Last updated on Oct 24, 2015

Get the free Member Claim Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Claim Form
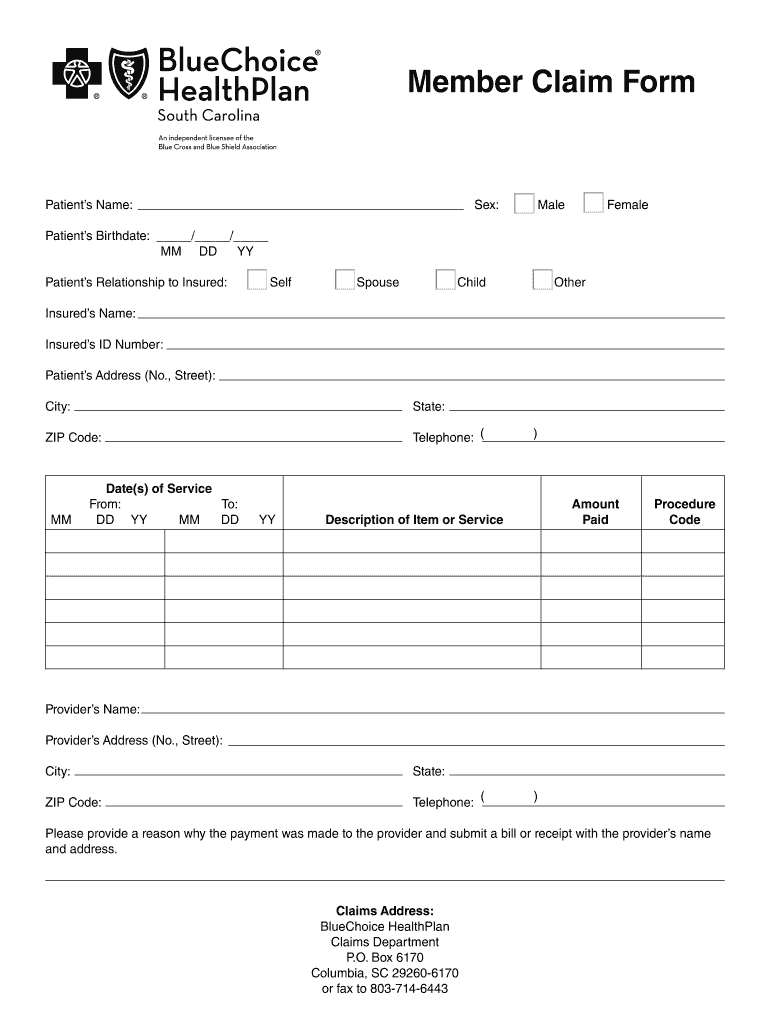
The Member Claim Form is a health insurance claim document used by patients to submit claims for medical services to BlueChoice HealthPlan.
pdfFiller scores top ratings on review platforms




Who needs Claim Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Claim Form
What is the Member Claim Form?
The Member Claim Form is a crucial document used by patients to submit health insurance claims to BlueChoice HealthPlan. This form allows patients to provide necessary information regarding their medical services, facilitating the reimbursement process. Essential requirements include the completion of all relevant fields to ensure efficient claim processing.
Purpose and Benefits of the Member Claim Form
This form is essential for patients aiming to secure reimbursement for medical expenses. By submitting claims using the Member Claim Form, patients can experience advantages such as enhanced processing times and increased chances of claim approval. Timely submissions significantly impact the efficiency of reimbursements, leading to quicker resolutions of outstanding claims.
Key Features of the Member Claim Form
The Member Claim Form contains numerous fillable fields that capture critical details necessary for claim approval. Key sections include:
-
Patient and insured information
-
Dates of service
-
Procedures performed and associated costs
-
Provider details for verification
-
Checkboxes for demographic information, including sex
Who Needs the Member Claim Form?
This form is designed for individuals who have received medical treatment covered under their health insurance. Eligible users include patients themselves, as well as dependents covered by the insured's policy. Understanding the distinction between insured individuals and patients is critical, especially in cases involving family members' healthcare needs.
How to Fill Out the Member Claim Form Online (Step-by-Step)
Filling out the Member Claim Form online is straightforward when using pdfFiller. Follow these steps to ensure a smooth process:
-
Access the form through pdfFiller.
-
Fill in each required field, including patient and insured details.
-
Provide accurate dates of service and amounts charged.
-
Review the completed form for completeness and accuracy.
-
Submit the form directly through the platform or save it for later submission.
Prior to starting, gather all necessary documentation such as bills and insurance information to assist in the process.
Submission Methods and Delivery
Once the Member Claim Form is completed, it can be submitted through various methods, ensuring flexibility for patients. Options include:
-
Online submission via pdfFiller
-
Sending the completed form by mail to the Claims Department in Columbia, South Carolina
-
Faxing the form if preferred
After submission, expect a processing period during which your claim will be reviewed and resolved.
Common Errors and How to Avoid Them
To prevent delays in processing the Member Claim Form, be aware of common errors that can occur. Frequent mistakes include:
-
Leaving mandatory fields empty
-
Submitting incorrect or mismatched information
-
Failing to sign and date the form
Utilize a checklist to confirm that all information is accurate before submission. If mistakes occur post-filing, familiarize yourself with the amendment process to correct errors efficiently.
Security and Compliance When Using the Member Claim Form
When using pdfFiller to complete the Member Claim Form, users can rest assured that their data is secure. pdfFiller employs 256-bit encryption and adheres to HIPAA compliance, ensuring the confidentiality of sensitive medical information. Understanding data handling policies is essential for safeguarding user rights throughout the claims process.
How to Use pdfFiller to Fill Out the Member Claim Form
Utilizing pdfFiller for the Member Claim Form enhances user experience considerably. Key advantages include:
-
The ability to edit and sign documents easily
-
Access to additional features for form management, such as saving and sharing
-
Encouragement to create an account for extended functionalities
This platform simplifies the claims process, making it more efficient for users.
Next Steps After Submitting the Member Claim Form
After submitting the Member Claim Form, you can expect a specified processing timeline for your claims. To keep track of your submission, check the status regularly. If a claim is rejected, or if further corrections are needed, follow the indicated procedures for resubmission or appeal.
How to fill out the Claim Form
-
1.Access the Member Claim Form by visiting pdfFiller and entering 'Member Claim Form' in the search bar to locate the document.
-
2.Open the form and review the fillable fields. Familiarize yourself with the sections that need to be completed.
-
3.Before starting, gather necessary information such as the patient’s name, birthdate, insured’s details, dates of service, procedure descriptions, and provider information.
-
4.Begin filling out the form by entering the patient’s name in the designated field, followed by their birthdate.
-
5.Complete the fields for the insured’s name and ID number. Ensure the information is accurate and corresponds with your insurance card.
-
6.Fill in the patient’s address details, including city, state, and ZIP code, followed by a contact telephone number.
-
7.Proceed to the 'Date(s) of Service' field. Enter all applicable dates when services were rendered.
-
8.In the 'Procedure Description' field, provide a brief summary of the services received. Be specific to avoid confusion during processing.
-
9.Enter the provider’s details, including their name, address, and telephone number, in the corresponding fields.
-
10.As you fill out the form, make use of checkboxes for 'Sex' and 'Patient’s Relationship to Insured' to ensure all required information is captured.
-
11.Once all sections are complete, review the entire form for accuracy. Cross-check the entered information against your records.
-
12.Finalize the form by clicking on the 'Save and Download' option in pdfFiller to store a copy for your records.
-
13.If you're ready to submit, follow the submission guidelines provided on the form, which may specify mailing instructions.

Who is eligible to use the Member Claim Form?
The Member Claim Form can be used by patients who have received medical services covered under their BlueChoice HealthPlan insurance. Family members listed as dependents are also eligible to submit claims using this form.
What supporting documents are required when submitting the claim?
When submitting the Member Claim Form, be sure to include any relevant receipts, itemized bills from the service provider, and necessary proof of payment to support your claim submission.
Where should I submit the completed Member Claim Form?
The completed Member Claim Form should be sent to the Claims Department in Columbia, South Carolina. Check your insurance policy for any additional submission methods, like online or fax options.
What are common mistakes to avoid when filling out the form?
Common mistakes include providing incomplete information, inaccuracies in the insured’s ID number, and failing to sign the form. Ensure all fields are filled accurately to prevent claim delays.
Are there deadlines for submitting the Member Claim Form?
Yes, there are generally specific deadlines for submitting claims. Check your BlueChoice HealthPlan policy for exact timelines to avoid your claim being denied due to late submission.
How long does it take to process a claim submitted with this form?
Processing times can vary depending on the complexity of the claim and the claims department's workload. Typically, expect to wait a few weeks, but check with BlueChoice for specific timelines.
Can I submit claims for multiple services on one form?
Yes, you can list multiple services on the same Member Claim Form, but be sure to provide accurate descriptions and dates of service for each to avoid confusion during processing.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.