Last updated on Oct 25, 2015
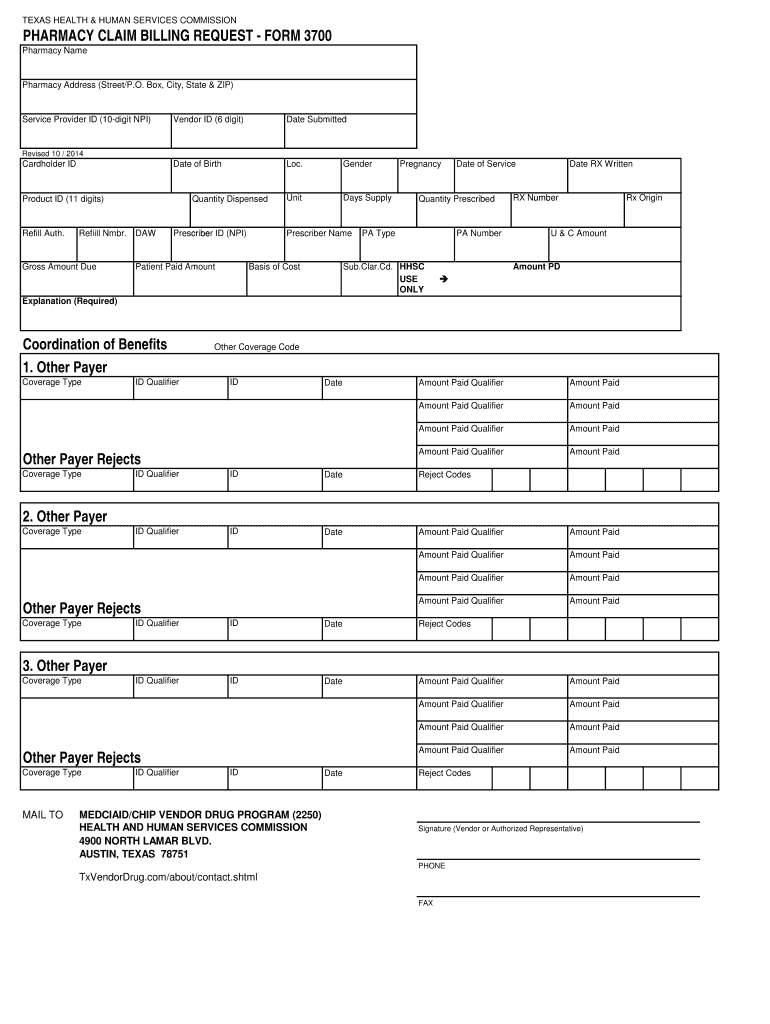

Get the free Texas Medicaid/CHIP Pharmacy Claims Billing Request
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Pharmacy Claims Billing Request
The Texas Medicaid/CHIP Pharmacy Claims Billing Request is a medical billing document used by healthcare providers to submit claims to the Texas Medicaid/CHIP Vendor Drug Program.
pdfFiller scores top ratings on review platforms




Who needs Pharmacy Claims Billing Request?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Pharmacy Claims Billing Request
What is the Texas Medicaid/CHIP Pharmacy Claims Billing Request?
The Texas Medicaid/CHIP Pharmacy Claims Billing Request, also known as Form 3700, is designed to facilitate the submission of paper claims for the Texas Medicaid and CHIP programs. This form is crucial when healthcare providers need to request reimbursements for pharmacy services, especially in circumstances such as natural disasters when electronic submissions may be inaccessible. Properly utilizing this form ensures a timely response from the relevant Texas authorities.
This form serves as an essential tool for maintaining compliance with regulations and expediting the claims process, making it an indispensable resource for healthcare providers within the system.
Purpose and Benefits of the Texas Medicaid/CHIP Pharmacy Claims Billing Request
The primary purpose of the Texas Medicaid/CHIP Pharmacy Claims Billing Request is to streamline the submission of pharmacy claims. By using this form, providers can ensure compliance with essential state regulations, which is critical for obtaining Medicaid and CHIP reimbursements. This can lead to quicker processing times for submitted claims.
Additionally, utilizing the correct billing form helps prevent unnecessary delays and denials, ultimately improving the financial performance of healthcare providers who serve Medicaid and CHIP clients.
Who Needs the Texas Medicaid/CHIP Pharmacy Claims Billing Request?
This form is necessary for healthcare providers who are enrolled in the Texas Medicaid and CHIP programs. Specifically, it is required for those providers who need to submit claims on behalf of their clients. Understanding the eligibility requirements for submission is vital to ensure that all claims are processed correctly.
Providers must be aware of the guidelines for submitting claims to qualify for reimbursement effectively. Each submission must align with the necessary compliance standards to avoid rejection or delays.
How to Complete the Texas Medicaid/CHIP Pharmacy Claims Billing Request Online
Completing the Texas Medicaid/CHIP Pharmacy Claims Billing Request involves a straightforward online process. Here are the steps to guide you:
-
Access the online form through the designated platform.
-
Fill out all required fields, including client identification and prescription details.
-
Ensure accurate entry of billing information to avoid errors.
-
Review the form for completeness before submission, emphasizing the need to sign and date it.
By following these steps closely, providers can enhance the accuracy and efficiency of their claims submissions.
Field-by-Field Instructions for the Texas Medicaid/CHIP Pharmacy Claims Billing Request
The form contains several key sections that need to be filled out accurately for successful processing. Here is an overview of the information required:
-
Client identification: Full name, Medicaid ID number, and other personal information.
-
Prescription details: Medication name, dosage, and fill date.
-
Billing information: Provider’s details, service dates, and total charges.
It is also crucial to understand how to properly utilize any checkboxes and optional fields to minimize the risk of common errors during form completion.
Submission Methods for the Texas Medicaid/CHIP Pharmacy Claims Billing Request
Submitting the completed Texas Medicaid/CHIP Pharmacy Claims Billing Request can be done through various methods. The main submission options include:
-
Mailing the completed form to the specified address.
-
Faxing the form directly to the Medicaid or CHIP office.
It's essential to adhere to submission deadlines to avoid penalties. Providers should also inquire about confirmation methods to track the status of their submissions once sent.
What Happens After You Submit the Texas Medicaid/CHIP Pharmacy Claims Billing Request?
After submission, Texas Medicaid/CHIP undertakes several steps to process the claim. Providers can check their claim status by following a specified procedure outlined by the program. Understanding common reasons for claim rejection is also vital to rectify issues promptly.
Being proactive in checking status and addressing potential concerns can vastly improve the claims experience for providers and clients alike.
Security and Compliance When Using the Texas Medicaid/CHIP Pharmacy Claims Billing Request
When handling sensitive health information using the Texas Medicaid/CHIP Pharmacy Claims Billing Request, security is of utmost importance. It is crucial to utilize secure methods for form submission to protect client data. Compliance with HIPAA and GDPR regulations ensures that all health information is managed securely.
Additionally, providers must be aware of the record retention requirements, which mandate keeping submitted forms for five years after the end of the federal fiscal year.
How pdfFiller Can Help You with the Texas Medicaid/CHIP Pharmacy Claims Billing Request
pdfFiller offers features that simplify the completion of the Texas Medicaid/CHIP Pharmacy Claims Billing Request. Providers can edit and fill out the form directly through a cloud-based platform, ensuring accessibility and ease of use. The platform also supports secure saving and eSigning, which streamlines the entire process.
Using pdfFiller enhances the overall experience for providers filling out necessary forms, leveraging technology for efficient document management.
Sample Completed Texas Medicaid/CHIP Pharmacy Claims Billing Request
A sample completed Texas Medicaid/CHIP Pharmacy Claims Billing Request showcases how to accurately fill out the required fields. Reviewing this completed form provides clarity on all necessary components and serves as a practical guide.
Providers are encouraged to download a blank version from pdfFiller and practice their filling skills using the example as a reference.
How to fill out the Pharmacy Claims Billing Request
-
1.Begin by visiting pdfFiller and search for 'Texas Medicaid/CHIP Pharmacy Claims Billing Request' to access the form.
-
2.Once the form is open, familiarize yourself with the layout and the fields that need to be completed.
-
3.Before filling out the form, gather necessary information such as client identification, prescription details, and billing information.
-
4.Using pdfFiller’s tools, click on the fields to enter the required client information accurately.
-
5.Ensure that all prescription information is precise, including medication names, quantities, and prescribing details.
-
6.Proceed to the billing sections, inputting relevant billing identifiers and ensure all information aligns with your client records.
-
7.Double-check the entered data for accuracy and completeness before finalizing the form.
-
8.After completing the form, review all fields to confirm no mistakes or omissions are present.
-
9.Utilize the 'Save' feature to keep a digital copy of the document on pdfFiller.
-
10.To submit the form, choose the appropriate option on pdfFiller to download it or send it electronically as specified by the Texas Medicaid/CHIP program.

Who is eligible to use the Texas Medicaid/CHIP Pharmacy Claims Billing Request?
This form is intended for healthcare providers and pharmacies that bill the Texas Medicaid/CHIP Vendor Drug Program, particularly for clients participating in these programs.
What types of claims can be submitted using this form?
This form is specifically designed for submitting paper claims related to pharmacy services under Medicaid and CHIP, including cases arising from natural disasters.
What is the deadline for submitting this form?
While specific deadlines can vary, it's typically required to submit pharmacy claims promptly after services are rendered, especially for time-sensitive cases like natural disasters.
Are there any supporting documents required with this form?
Yes, supporting documents may be required depending on the claim specifics, including prescriptions and proof of client eligibility for Medicaid/CHIP.
How can I avoid common mistakes when filling out this form?
Ensure accuracy by double-checking client information and prescription details, confirming that all necessary fields are filled out, and validating that the form is signed and dated.
What is the processing time for claims submitted with this form?
Processing times for claims can vary; however, claims are generally processed within a few weeks, depending on the completeness of the documentation provided.
Can this form be submitted electronically?
While this form may be completed electronically through pdfFiller, the submission method must adhere to Texas Medicaid/CHIP guidelines which may require the forms to be printed and mailed.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.