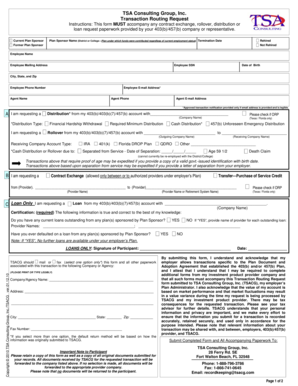Last updated on Oct 25, 2015

Get the free Automatic Premium Payment Authorization Agreement
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Premium Payment Authorization
The Automatic Premium Payment Authorization Agreement is a healthcare form used by Blue Cross Medicare Advantage members to authorize automatic monthly withdrawals for insurance premium payments.
pdfFiller scores top ratings on review platforms




Who needs Premium Payment Authorization?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Premium Payment Authorization
What is the Automatic Premium Payment Authorization Agreement?
The Automatic Premium Payment Authorization Agreement is a crucial healthcare form for Blue Cross Medicare Advantage members in Pennsylvania. Its primary purpose is to enable members to authorize automatic monthly premium payments, ensuring that payments are made on time without the need for manual intervention. This agreement falls under the category of healthcare forms, facilitating easier management of insurance premiums for members and their families.
Purpose and Benefits of Automatic Premium Payment Authorization
The agreement serves several key purposes for its members and account holders. It primarily allows for automated payments, providing a hassle-free approach to manage insurance premiums. This automation translates to convenience, ensuring timely payments which are essential for continuous healthcare access. Members can focus more on their health and less on payment schedules, thereby enhancing financial management and peace of mind.
Who Needs the Automatic Premium Payment Authorization Agreement?
The target audience for this agreement includes Blue Cross Medicare Advantage members and their account holders residing in Pennsylvania. Both the member and account holder must sign the agreement, as joint authorization is often necessary to validate the payment process. Additionally, guardians or family members who oversee financial matters may need to be involved, ensuring all parties are aligned on the payment arrangements.
How to Fill Out the Automatic Premium Payment Authorization Agreement Online
Filling out the Automatic Premium Payment Authorization Agreement online can be straightforward by following these steps:
-
Access pdfFiller’s platform to locate the agreement form.
-
Gather necessary personal and financial information, including a voided check.
-
Carefully enter the required details into the provided fields.
-
Review the form to ensure accuracy, paying special attention to member and banking information.
-
Sign the document electronically before submission.
Ensure you familiarize yourself with common areas that may cause errors, which can prolong the processing time.
Field-by-Field Instructions for the Automatic Premium Payment Authorization Agreement
To successfully complete the Automatic Premium Payment Authorization Agreement, it is essential to understand each section. Key fields include:
-
Member details: Full name and ID number.
-
Bank information: Account number and routing number.
-
Signature areas: Both member and account holder signatures.
Visual aids or examples within the pdfFiller platform can further clarify how to fill out specific sections correctly.
Submission Methods for the Automatic Premium Payment Authorization Agreement
Members can submit the completed Automatic Premium Payment Authorization Agreement through several methods:
-
Online via pdfFiller for immediate processing.
-
Mail, but ensure to use a tracked envelope for security.
For users in Pennsylvania, there may be specific submission guidelines to follow, which can be accessed on the official website.
Security and Compliance Considerations for the Automatic Premium Payment Authorization Agreement
As the Automatic Premium Payment Authorization Agreement includes sensitive personal information, security is paramount. This document adheres to compliance regulations such as HIPAA and GDPR, ensuring your privacy is protected. pdfFiller implements 256-bit encryption to safeguard your data during submission and storage, allowing members to confidently manage their healthcare forms online.
What Happens After You Submit the Automatic Premium Payment Authorization Agreement?
Upon submission of the Automatic Premium Payment Authorization Agreement, members can expect the following:
-
Confirmation of receipt via email or through the platform.
-
A processing timeline that typically spans a few business days.
-
Instructions on how to check the status of your authorization, should follow-up be necessary.
How to Correct or Amend the Automatic Premium Payment Authorization Agreement
Should there be any errors after submitting the Automatic Premium Payment Authorization Agreement, it is essential to correct inaccuracies promptly. Members can make amendments by contacting customer support or re-submitting a corrected form. Accurate information is crucial as any discrepancies may delay payment processing and affect healthcare access.
Enhance Your Experience with pdfFiller for the Automatic Premium Payment Authorization Agreement
Utilizing pdfFiller provides an enhanced user experience when managing the Automatic Premium Payment Authorization Agreement. This cloud-based platform enables secure editing, filling, and submission of forms. It offers features such as eSigning, easy sharing options, and robust document security to streamline the process for healthcare insurance forms.
How to fill out the Premium Payment Authorization
-
1.Access pdfFiller and log in or create an account if you don't have one.
-
2.Search for 'Automatic Premium Payment Authorization Agreement' in the form library.
-
3.Open the form to view the editable PDF.
-
4.Familiarize yourself with the document by reviewing instructions at the top of the form.
-
5.Prepare your personal and financial information including bank details and identification.
-
6.Fill in the required fields, including your name, contact information, and account details.
-
7.Use the checkboxes provided to indicate your agreement to the terms stated.
-
8.Attach a voided check as instructed for payment authorization verification.
-
9.Review all entered information for accuracy to avoid processing delays.
-
10.Save your progress on pdfFiller by clicking on the 'Save' button at the top.
-
11.Download your completed form or submit directly through pdfFiller if required.

Who is eligible to fill out the Automatic Premium Payment Authorization Agreement?
This form is primarily intended for Blue Cross Medicare Advantage members and account holders who want to set up automatic premium payments. Eligibility may also depend on residency in specific states like Pennsylvania.
What information do I need to complete this form?
Before filling out the Automatic Premium Payment Authorization Agreement, gather your personal details, financial information including bank account number, routing number, and identification, as well as a voided check for verification.
How do I submit the completed form?
Completed forms can typically be submitted online through pdfFiller or printed and mailed to the appropriate address as indicated in the form instructions. Always check submission methods to ensure adherence to guidelines.
What are common errors to avoid when filling out this form?
Common mistakes include missing signatures, providing incorrect bank account information, and neglecting to attach a voided check. Always double-check all filled information before submission.
Is notarization required for this form?
No, the Automatic Premium Payment Authorization Agreement does not require notarization, simplifying the process for users.
Are there any processing fees associated with this form?
Typically, there are no fees specifically associated with filling out this form. However, always verify with your insurance provider for any related costs.
How long does it take for automatic payments to start after submitting this form?
Once submitted, automatic premium payments usually begin within one or two billing cycles. It’s advisable to confirm with your insurance provider for specific timelines.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.