Last updated on Oct 27, 2015

Get the free Ohana Health Plan Coverage Determination Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Coverage Determination Request
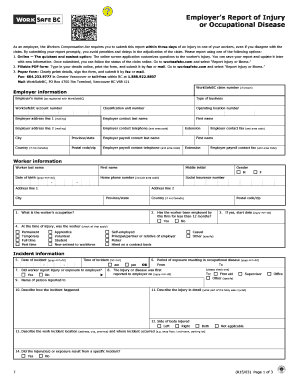
The Ohana Health Plan Coverage Determination Request Form is a medical consent form used by healthcare providers to determine coverage for prior authorizations and medications.
pdfFiller scores top ratings on review platforms




Who needs Coverage Determination Request?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Coverage Determination Request
What is the Ohana Health Plan Coverage Determination Request Form?
The Ohana Health Plan Coverage Determination Request Form is a critical document in the healthcare sector, particularly utilized for prior authorizations and medication coverage. It serves to facilitate the approval of medications and treatments, ensuring that patient care remains uninterrupted. This form requires the compilation of essential information, including member data and physician details, to support coverage decisions under utilization management guidelines.
Purpose and Benefits of the Ohana Health Plan Coverage Determination Request Form
This form is invaluable for both patients and healthcare providers. It streamlines the process of obtaining necessary medications by reducing administrative burdens and facilitating timely approvals. By fostering efficiency and clarity in the prior authorization process, the Ohana Health Plan Coverage Determination Request Form alleviates potential delays, benefiting all parties involved.
Among the key advantages are:
-
Enhanced communication between healthcare providers and insurance companies
-
Faster access to prescribed medications for patients
-
Increased transparency in the medication coverage process
Key Features of the Ohana Health Plan Coverage Determination Request Form
This form boasts several essential attributes necessary for its effectiveness. Required fields include:
-
Member information such as name and date of birth
-
Physician details, including contact information and licensure
-
Medication specifics, including dosage and frequency
Additionally, the inclusion of a clinical rationale is crucial as it directly impacts the outcome of coverage decisions. Ensuring accuracy in these sections is vital for a successful submission.
Who Needs the Ohana Health Plan Coverage Determination Request Form?
The primary audience for the Ohana Health Plan Coverage Determination Request Form includes physicians and authorized personnel who are responsible for managing patient care. The form must be filled out accurately, and it is essential that it bears a physician's signature to validate the request. This requirement ensures that all requests are medically justified and comply with regulatory standards.
How to Fill Out the Ohana Health Plan Coverage Determination Request Form Online (Step-by-Step)
Completing the Ohana Health Plan Coverage Determination Request Form online can be accomplished by following these steps:
-
Access the form through your preferred PDF editing platform.
-
Fill in the member information accurately, ensuring to include all required details.
-
Provide the physician's information and ensure it is complete.
-
Detail the specific medication being requested, along with the clinical rationale.
-
Review all entries for accuracy before finalizing the form.
-
Submit the form through the designated channels as instructed.
Gathering necessary information beforehand can increase efficiency and help in reducing errors while completing the form.
Common Errors to Avoid When Completing the Ohana Health Plan Coverage Determination Request Form
To ensure a smooth submission process, users should be aware of common errors that can lead to rejection of the request:
-
Omitting crucial fields, such as member or physician information
-
Failing to provide a valid clinical rationale
-
Errors in medication details, including dosage and frequency
Before submission, double-checking the form for such inaccuracies can help prevent delays in medication approval.
Submission Methods for the Ohana Health Plan Coverage Determination Request Form
Once completed, the Ohana Health Plan Coverage Determination Request Form can be submitted through various methods. The primary submission option is faxing the form directly to WellCare’s Pharmacy Department. Tracking the submission and obtaining confirmation is important to ensure that the request is processed in a timely manner.
Security and Compliance When Using the Ohana Health Plan Coverage Determination Request Form
Privacy and data protection are paramount when handling sensitive information via the Ohana Health Plan Coverage Determination Request Form. Compliance with HIPAA regulations safeguards patient data, ensuring confidentiality and security. Using a secure platform, such as pdfFiller, adds an extra layer of protection, utilizing robust security features to protect personal health information.
Utilizing pdfFiller for the Ohana Health Plan Coverage Determination Request Form
pdfFiller offers a comprehensive set of tools designed to simplify the completion of the Ohana Health Plan Coverage Determination Request Form. Users can take advantage of features such as eSigning and form editing to enhance functionality. Utilizing pdfFiller ensures that users can complete and submit their forms efficiently, without the need for complex software installations.
Next Steps After Submitting the Ohana Health Plan Coverage Determination Request Form
After submitting the form, it is important to track the application status and remain informed about expected processing times. If corrections or amendments are necessary, users should follow the designated procedures outlined by their healthcare provider or insurance company. Regular updates will help manage expectations regarding medication availability.
How to fill out the Coverage Determination Request
-
1.To access the Ohana Health Plan Coverage Determination Request Form on pdfFiller, visit the website and search for the form by its name.
-
2.Open the form in pdfFiller’s editor interface. Familiarize yourself with the layout and available tools.
-
3.Gather necessary information, including member details, physician information, specific medication, and clinical rationale before starting your completion.
-
4.Begin by filling in the member's information in the designated fields such as 'Member Name' and 'Date of Request'.
-
5.Next, complete the physician's details, especially ensuring that the physician's signature field is left open for review.
-
6.Use checkboxes and text fields where applicable to provide details regarding the medication's specifics and the rationale for the request.
-
7.Once all fields are completed, review the form for any missing information or potential errors. Check that all required fields are properly filled.
-
8.After reviewing, finalize the document by saving your work within pdfFiller.
-
9.Download or submit the form as directed—ensure it is faxed to WellCare’s Pharmacy Department while adhering to HIPAA privacy regulations.

Who is eligible to submit the Ohana Health Plan Coverage Determination Request Form?
Eligible submitters include licensed healthcare providers like physicians who manage patients under the Ohana Health Plan needing medication prior authorization.
Are there deadlines for submitting this coverage determination request?
While specific deadlines may vary, it's best to submit requests promptly to prevent delays in medication access. Check specific plan rules for exact timelines.
How do I submit the completed form?
The completed form should be faxed to WellCare’s Pharmacy Department. Ensure you retain a copy for your records.
What supporting documents are required with this form?
Supporting documents may include medical records, prior treatment details, and insurance information to justify the medication request. Check with the plan for specifics.
What common mistakes should I avoid when completing this form?
Common mistakes include omitting required fields, failing to obtain the necessary physician signature, and not double-checking for accuracy before submission.
What is the typical processing time for this coverage determination request?
Processing times can vary; however, most requests should receive a response within a few days. Contact the pharmacy department for specific inquiries.
Is this form mandatory for all medication requests?
Yes, this form is usually mandatory for medications that require prior authorization under the Ohana Health Plan. Always confirm specific requirements with the plan.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.