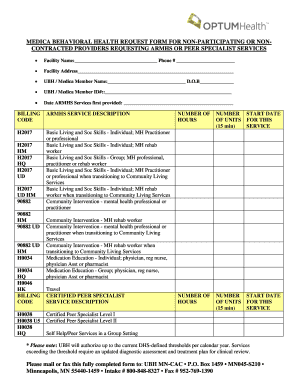
Last updated on Aug 19, 2013

Get the free Medical Assistance Program Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is medical assistance program prior
The Medical Assistance Program Prior Authorization Request Form is a healthcare document used by agencies to request prior authorization for specific medical services.
pdfFiller scores top ratings on review platforms




Who needs medical assistance program prior?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to medical assistance program prior
What is the Medical Assistance Program Prior Authorization Request Form?
The Medical Assistance Program Prior Authorization Request Form is essential for initiating prior authorization for various healthcare services. This form plays a critical role in ensuring that necessary services like Private Duty Nursing, Long Term Home Health, and EPSDT Extraordinary Home Health are covered under the medical assistance program. To complete the form effectively, specific client information and supporting documentation are required.
Key information includes the patient's demographics, service codes, and any relevant medical history. Understanding the purpose of this form aids healthcare providers and patients alike in navigating the complexities of Colorado's healthcare system.
Purpose and Benefits of the Medical Assistance Program Prior Authorization Request Form
The Medical Assistance Program Prior Authorization Request Form simplifies the process of securing necessary healthcare services through prior authorization. This form ensures that patients receive coverage for essential treatments, which can lead to improved health outcomes. Additionally, it helps streamline communication between healthcare providers and patients, reducing administrative burdens.
-
Using this form can expedite the authorization process, ensuring timely access to care.
-
It minimizes the risk of misunderstandings regarding service coverage, which can lead to delays.
-
Failure to utilize the form may result in potential denials or significant delays in receiving necessary services.
Who Needs the Medical Assistance Program Prior Authorization Request Form?
Various stakeholders are involved in the completion of the Medical Assistance Program Prior Authorization Request Form. This form should be filled out by healthcare providers, patients, or their designated representatives. The Requesting Agency & Representative and the Authorizing Party each play vital roles in the authorization process.
It is crucial that these individuals provide accurate information and correct signatures to avoid complications during approval, ensuring that the process runs smoothly and efficiently.
How to Fill Out the Medical Assistance Program Prior Authorization Request Form Online
Completing the Medical Assistance Program Prior Authorization Request Form online through pdfFiller is straightforward and user-friendly. To begin, access the form on the pdfFiller platform, where you'll find a fillable version ready for completion.
-
Begin by entering required client details in the designated fields.
-
Utilize checkboxes to select relevant services covered under the request.
-
Easily navigate to sections using intuitive form elements to enhance your experience.
-
The platform also offers an eSigning feature, allowing for seamless digital signatures.
Common Errors and How to Avoid Them When Filling Out the Form
When filling out the Medical Assistance Program Prior Authorization Request Form, users may encounter several common mistakes that can hinder processing. Typical errors include leaving fields incomplete or misinterpreting the provided instructions.
-
Thoroughly review each section before submission to ensure all required fields are completed accurately.
-
Double-check the information entered and cross-reference with your documentation.
-
A validation checklist can be useful to streamline the process and minimize oversights.
Submission Methods and Delivery Details for the Form
Once the Medical Assistance Program Prior Authorization Request Form is completed, it can be submitted through various methods. Options include online submissions via pdfFiller, mailing the form, or sending it via fax. Each method has its benefits based on user preferences.
-
Be mindful of any submission deadlines to ensure timely processing.
-
Check for confirmation of receipt after submission to track the status of your request.
-
Tracking options may be available depending on the chosen submission method.
What Happens After You Submit the Medical Assistance Program Prior Authorization Request Form
After the submission of the Medical Assistance Program Prior Authorization Request Form, a review process is initiated. Understanding what happens next can help users navigate expectations effectively.
-
The typical outcomes include approval, denial, or requests for additional information or clarification.
-
Stay informed about the status of your application and know the steps to take in case of a denial.
-
Being proactive in communication can facilitate faster resolution of issues that may arise.
Security and Compliance Considerations for Using the Form
Ensuring the safety of personal and health data while using the Medical Assistance Program Prior Authorization Request Form is paramount. The pdfFiller platform utilizes advanced security measures to protect sensitive information, including 256-bit encryption and compliance with both HIPAA and GDPR regulations.
-
Protecting health information is critical when handling sensitive documents, and pdfFiller emphasizes this commitment.
-
Familiarize yourself with data retention policies to ensure your information is managed securely.
-
Privacy concerns should always be at the forefront when collecting or transmitting sensitive data online.
Simplifying the Medical Assistance Program Prior Authorization Request Process with pdfFiller
pdfFiller offers numerous benefits that can simplify the Medical Assistance Program Prior Authorization Request process. With user-friendly features designed for ease of use, this platform allows users to create, edit, eSign, and securely store their forms all in one place.
-
Utilize tools for annotation and document management that enhance submission accuracy.
-
Hear from satisfied users who have successfully navigated the form-filling process with pdfFiller.
-
Experience the convenience of managing healthcare documents efficiently on a trusted platform.
How to fill out the medical assistance program prior
-
1.To access the Medical Assistance Program Prior Authorization Request Form on pdfFiller, visit the website and log in to your account or create a new account if you do not have one.
-
2.Once logged in, use the search bar to type in the form name or navigate through the 'Healthcare Forms' category to locate the form.
-
3.Click on the form to open it in the pdfFiller editor where you can navigate the fields easily using your mouse or keyboard.
-
4.Before starting, gather necessary information such as client identification details, service codes, and relevant documentation to ensure you’re prepared.
-
5.Fill in the required fields, ensuring all necessary client and service information is accurately entered; utilize the highlighting tools to guide your completion process.
-
6.Pay special attention to the areas requiring signatures, as both the requesting agency and the authorizing party need to provide their approval by signing the form.
-
7.When you've filled out the form completely, review all entries for accuracy to avoid common mistakes.
-
8.Utilize the 'Preview' option to see the filled form before finalizing to check for any missing information.
-
9.Once satisfied, save your completed form in your pdfFiller account for future access or download it as a PDF for submission.
-
10.To submit the form, you may either print it out and send it to the appropriate agency or submit it electronically through the designated method provided by the agency.

Who is eligible to use the Medical Assistance Program Prior Authorization Request Form?
This form is intended for healthcare providers and agencies that are seeking prior authorization for medical services such as Private Duty Nursing and Long Term Home Health. Ensure you represent an eligible agency or patient.
What services require prior authorization?
The services that typically require prior authorization using this form include Private Duty Nursing, Long Term Home Health, and EPSDT Extraordinary Home Health services as specified for Colorado.
How do I submit the completed form?
You can submit the completed Medical Assistance Program Prior Authorization Request Form by printing and mailing it to the appropriate agency or by submitting it electronically if instructed. Always check submission methods with the receiving agency.
Is there a deadline for submitting this prior authorization request?
Deadlines for submitting the prior authorization request depend on the specific service being requested and the agency’s policies. It is best to submit as soon as possible to avoid delays in service access.
What documents do I need to support the prior authorization request?
Typically, you will need client identification information, relevant service codes, and any necessary medical records or supporting documents that validate the need for the requested services.
What are common mistakes to avoid when filling out this form?
Common mistakes include missing required signatures, inaccurate or incomplete client information, and forgetting to include supporting documentation. Double-check all fields for completeness before submission.
How long does it take to process the prior authorization request?
Processing times vary by agency but generally range from a few days to several weeks. Check with the specific agency for more accurate time frames related to your request.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.