Last updated on Mar 27, 2026

CA DWC SBR-1 free printable template
pdfFiller is not affiliated with any government organization
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is CA DWC SBR-1
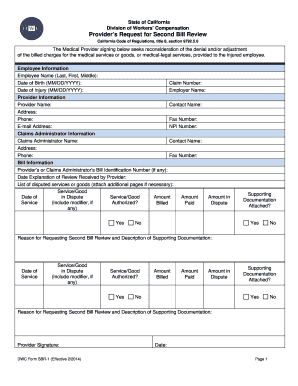
The California Provider’s Request for Second Bill Review is a medical billing form used by medical providers in California to dispute payments for treatment services or medical-legal expenses.
pdfFiller scores top ratings on review platforms




Good product at a good price.
This product works well.
Great customer service
Great customer service, such a hard thing to come across. Easy access to your cloud uploaded documents from any device. The only thing limiting the 5 star is the relatively clunky interface. Still would use again for secure pdf development.
Who needs CA DWC SBR-1?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to CA DWC SBR-1
What is the California Provider’s Request for Second Bill Review?
The California Provider’s Request for Second Bill Review, also known as DWC Form SBR-1, is essential for medical providers aiming to dispute underpayments for services rendered in workers' compensation cases. This document enables providers to contest the amounts paid by claims administrators for medical treatment or medical-legal expenses.
Disputing medical billing amounts is crucial in ensuring fair compensation for healthcare services. The regulations surrounding California workers' compensation emphasize the importance of accurate billing, making this form a vital tool for providers seeking to protect their revenue streams.
Purpose and Benefits of the California Provider’s Request for Second Bill Review
This form is crucial for medical providers as it helps ensure they receive fair compensation for their services. By utilizing this form, providers can effectively challenge underpayments or billing disputes that may arise.
Some of the benefits associated with using the California Provider’s Request for Second Bill Review include:
-
Facilitating the challenging of underpayments effectively.
-
Protecting the revenue cycle by addressing discrepancies in billing.
-
Enhancing the likelihood of receiving appropriate reimbursement for services provided.
Who Needs the California Provider’s Request for Second Bill Review?
Medical providers in California who accept workers' compensation cases are the primary users of this form. There are specific scenarios where the second bill review becomes necessary:
-
Instances of billing disputes with claims administrators.
-
When providers receive less compensation than expected for services rendered.
-
Cases requiring clarification and formal dispute for underpayments.
Eligibility criteria for utilizing this form include being a licensed medical provider engaged with workers' compensation claims.
When and How to Submit the California Provider’s Request for Second Bill Review
The California Provider’s Request for Second Bill Review must be submitted within 90 days of receiving the explanation of review from the claims administrator. Here are the steps to take when submitting the form:
-
Complete DWC Form SBR-1 with all requested details.
-
Attach any necessary supporting documentation related to the billing dispute.
-
Choose your submission method: online or via postal mail.
Required Documents and Information for the California Provider’s Request for Second Bill Review
To successfully complete the California Provider’s Request for Second Bill Review, several documents and pieces of information are required:
-
Patient information, including treatment dates and details.
-
Provider details, confirming their involvement and services.
-
Claims administrator information, essential for coordination.
-
All relevant parts of the disputed billing, such as amounts billed, paid, and in dispute.
It's important to attach supporting documents to substantiate the claims within the form.
How to Fill Out the California Provider’s Request for Second Bill Review Online
Filling out the form online can simplify the process. Here are field-by-field instructions to guide you:
-
Start by entering patient details accurately.
-
Provide information about the services rendered, ensuring correct dates and amounts.
-
Double-check every completed section to avoid common errors.
-
Attach all supporting documentation before final submission.
Tips for ensuring accuracy and completeness include reviewing all entries and confirming document attachments.
Checking the Status of Your California Provider’s Request for Second Bill Review
After submitting the California Provider’s Request for Second Bill Review, it's crucial to keep track of your submission. To check the status, follow these steps:
-
Use the claims administrator's online portal or contact them directly.
-
Be aware of common reasons for processing delays.
-
Maintain records of your submission for reference during inquiries.
This process helps ensure you stay informed regarding your billing disputes.
Security and Compliance of the California Provider’s Request for Second Bill Review
Your sensitive information's security is paramount when handling the California Provider’s Request for Second Bill Review. pdfFiller implements robust security measures, including:
-
256-bit encryption to protect all data during transmission.
-
Compliance with HIPAA and GDPR to safeguard personal health information.
Using a trusted platform like pdfFiller enhances the filing experience while ensuring user data privacy and document security.
Why Use pdfFiller for Submitting the California Provider’s Request for Second Bill Review?
Using pdfFiller for your California Provider’s Request for Second Bill Review offers several advantages. Users can benefit from:
-
Convenience in online form filling and eSigning.
-
Features that facilitate hassle-free editing, sharing, and managing of documents.
This user-friendly platform is designed with security in mind, making it the preferred choice for medical providers handling sensitive documents.
Get Started with Your California Provider’s Request for Second Bill Review Today!
Now that you understand the benefits of using pdfFiller, you can start the process of filling out the California Provider’s Request for Second Bill Review online. With secure document management and an easy-to-navigate interface, pdfFiller simplifies your billing dispute management.
How to fill out the CA DWC SBR-1
-
1.To access the California Provider’s Request for Second Bill Review on pdfFiller, visit the pdfFiller website and use the search function to locate the form by its official name.
-
2.Open the form and familiarize yourself with pdfFiller's interface, specifically noting where you can input text and where any checkboxes are located.
-
3.Before starting, gather all necessary information including the employee's details, provider's information, claims administrator's contact, and specifics about the disputed bill such as the date of service, billed amounts, and payment facts.
-
4.Begin filling out the form by clicking on the fields to enter the required information. Ensure each section is accurately completed to avoid delays in processing your request.
-
5.Indicate if you have attached supporting documentation by checking the appropriate box. Clearly state the reason for requesting the second bill review in the designated space.
-
6.After all fields are populated, take a moment to review the form for accuracy, ensuring all information is correct and any required signatures are present.
-
7.Once reviewed, you can save the form as a draft in pdfFiller or download it directly to your device. If you wish to submit it electronically, follow the procedure provided by pdfFiller for direct submission to the claims administrator.

Who is eligible to use the California Provider’s Request for Second Bill Review?
Medical providers in California who have received a payment they believe is incorrect for treatment services can use this form to initiate a second bill review.
What is the deadline for submitting the form?
The form must be submitted to the claims administrator within 90 days of receiving the explanation of review to ensure timely processing.
How do I submit the completed form?
Once completed, you may either submit the form via pdfFiller directly to the claims administrator or download it and send it by mail, depending on their submission preferences.
Are supporting documents required with this form?
Yes, it is important to attach any supporting documentation that substantiates the billing dispute, and check the box indicating that these documents are included.
What mistakes should I avoid when filling out the form?
Be careful not to leave any fields blank and thoroughly check for accuracy in all dates, amounts, and signatures to avoid delays in processing your request.
How long does it take to process the request after submission?
Processing times may vary depending on the claims administrator's procedures, but it typically takes several weeks to receive a response after submission.
What if I have further questions about the bill review process?
For more detailed inquiries, consider contacting the claims administrator directly or consulting with a legal professional familiar with workers' compensation and billing disputes.
Related Catalogs
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.