
Get the free 800 314 6223
Show details
Pharmacy Prior Authorization Form ? Fax Completed Form to (800) 314-6223 PA forms and guidelines are available on the provider portal of www.healthnet.com If the fax number provided is not a dedicated
We are not affiliated with any brand or entity on this form
Get, Create, Make and Sign 800 314 6223 form
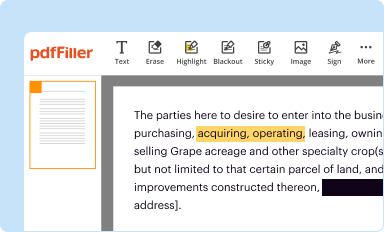
Edit your 800 314 6223 form online
Type text, complete fillable fields, insert images, highlight or blackout data for discretion, add comments, and more.
Add your legally-binding signature
Draw or type your signature, upload a signature image, or capture it with your digital camera.

Share your form instantly
Email, fax, or share your 800 314 6223 form via URL. You can also download, print, or export forms to your preferred cloud storage service.
Editing 800 314 6223 online
Follow the steps down below to benefit from a competent PDF editor:
1
Create an account. Begin by choosing Start Free Trial and, if you are a new user, establish a profile.
2
Upload a file. Select Add New on your Dashboard and upload a file from your device or import it from the cloud, online, or internal mail. Then click Edit.
3
Edit 800 314 6223. Text may be added and replaced, new objects can be included, pages can be rearranged, watermarks and page numbers can be added, and so on. When you're done editing, click Done and then go to the Documents tab to combine, divide, lock, or unlock the file.
4
Get your file. Select your file from the documents list and pick your export method. You may save it as a PDF, email it, or upload it to the cloud.
pdfFiller makes dealing with documents a breeze. Create an account to find out!
Uncompromising security for your PDF editing and eSignature needs
Your private information is safe with pdfFiller. We employ end-to-end encryption, secure cloud storage, and advanced access control to protect your documents and maintain regulatory compliance.
How to fill out 800 314 6223
How to fill out 800 314 6223?
01
Begin by dialing the numbers "800" on your phone's keypad.
02
Follow it by entering the numbers "314" on your phone's keypad.
03
Complete the phone number by dialing the final digits "6223" on your phone's keypad.
Who needs 800 314 6223?
01
Individuals who are looking for customer support assistance from a particular company or organization may need to contact 800 314 6223.
02
Those who have inquiries, issues, or require assistance related to a product or service may find it necessary to call this phone number.
03
Customers who need to speak with a representative regarding billing, technical support, placing orders, or any other relevant matters may also utilize 800 314 6223 to get the necessary help.
Fill
form
: Try Risk Free






For pdfFiller’s FAQs
Below is a list of the most common customer questions. If you can’t find an answer to your question, please don’t hesitate to reach out to us.
How can I edit 800 314 6223 from Google Drive?
It is possible to significantly enhance your document management and form preparation by combining pdfFiller with Google Docs. This will allow you to generate papers, amend them, and sign them straight from your Google Drive. Use the add-on to convert your 800 314 6223 into a dynamic fillable form that can be managed and signed using any internet-connected device.
How do I fill out the 800 314 6223 form on my smartphone?
You can quickly make and fill out legal forms with the help of the pdfFiller app on your phone. Complete and sign 800 314 6223 and other documents on your mobile device using the application. If you want to learn more about how the PDF editor works, go to pdfFiller.com.
How can I fill out 800 314 6223 on an iOS device?
In order to fill out documents on your iOS device, install the pdfFiller app. Create an account or log in to an existing one if you have a subscription to the service. Once the registration process is complete, upload your 800 314 6223. You now can take advantage of pdfFiller's advanced functionalities: adding fillable fields and eSigning documents, and accessing them from any device, wherever you are.
What is 800 314 6223?
800 314 6223 is the phone number for the Internal Revenue Service (IRS) taxes hotline.
Who is required to file 800 314 6223?
No one is required to file 800 314 6223. It is a phone number for inquiring about tax-related information.
How to fill out 800 314 6223?
There is no specific form or process to fill out 800 314 6223. You simply dial the phone number to reach the IRS taxes hotline.
What is the purpose of 800 314 6223?
The purpose of 800 314 6223 is to provide taxpayers with a hotline to inquire about tax-related information and get assistance from the IRS.
What information must be reported on 800 314 6223?
No information needs to be reported on 800 314 6223. It is a phone number to seek information from the IRS.
Fill out your 800 314 6223 online with pdfFiller!
pdfFiller is an end-to-end solution for managing, creating, and editing documents and forms in the cloud. Save time and hassle by preparing your tax forms online.

800 314 6223 is not the form you're looking for?Search for another form here.
Relevant keywords
Related Forms
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.





















