Last updated on Apr 10, 2026

Cigna Uniform Pharmacy Prior Authorization Request free printable template
pdfFiller is not affiliated with any government organization
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Cigna Uniform Pharmacy Prior Authorization Request
The Pharmacy Prior Authorization Request Form is a healthcare document used by prescribers to request prior authorization for prescription medications.
pdfFiller scores top ratings on review platforms




Who needs Cigna Uniform Pharmacy Prior Authorization Request?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Cigna Uniform Pharmacy Prior Authorization Request
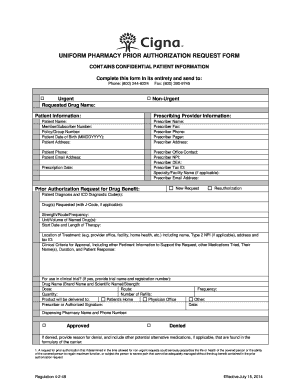
What is the Pharmacy Prior Authorization Request Form?
The Pharmacy Prior Authorization Request Form is an essential document used by healthcare providers to obtain approvals for specific prescription medications. This form plays a crucial role in ensuring that prescribed drugs are necessary and aligned with clinical criteria. Proper completion of the form requires detailed information such as patient data, prescriber details, and relevant clinical information.
Healthcare providers must ensure that all required fields are filled correctly, as incomplete forms can delay the authorization process. Information such as patient demographics and prescription specifics must be accurately documented to facilitate timely decisions regarding medical treatments.
Purpose and Benefits of the Pharmacy Prior Authorization Request Form
This request form streamlines the medication approval process, enabling faster access to needed therapies for patients. By using a standardized format, healthcare providers can efficiently communicate the clinical rationale for prescriptions, thus improving patient care.
Additionally, the implementation of this form aids in cost management for healthcare providers, allowing for better oversight of prescription medications. This proactive approach results in both better healthcare outcomes and enhanced patient satisfaction.
Who Needs the Pharmacy Prior Authorization Request Form?
The primary users of the Pharmacy Prior Authorization Request Form are prescribers and dispensing pharmacies. It is an indispensable tool for healthcare professionals who aim to secure medication approvals for their patients.
Various healthcare providers across specialties may require this form to navigate complex authorization processes, ensuring that patients receive their prescribed therapies without unnecessary delays.
Key Features of the Pharmacy Prior Authorization Request Form
The form contains multiple fillable fields and sections designed to facilitate completion. Each element is crucial, from patient identifiers to prescription details, ensuring comprehensive documentation of the medical necessity for the prescribed drugs.
Prescribers must sign the form, indicating verification of its contents before submission. Understanding the submission process is equally important, as it guides users on how to effectively send the completed form to the appropriate authorities.
How to Fill Out the Pharmacy Prior Authorization Request Form Online
To complete the form online using pdfFiller, follow these straightforward steps:
-
Access the form on the pdfFiller platform.
-
Gather necessary details such as patient information and drug specifics.
-
Fill in each section accurately, ensuring all required fields are completed.
-
Review the form for accuracy and completeness.
-
Submit the form electronically through the provided channels.
Having the right information prior to form completion can significantly streamline the process and minimize errors.
Submission Methods for the Pharmacy Prior Authorization Request Form
There are several submission methods available for the completed Pharmacy Prior Authorization Request Form. These options may include:
-
Faxing the form to the designated number.
-
Sending the form via secure email to the intended recipient.
-
Utilizing online submission portals where applicable.
Understanding where to send the form is crucial, along with awareness of any potential fees associated with submission methods.
Common Errors and How to Avoid Them
When filling out the Pharmacy Prior Authorization Request Form, users often encounter common mistakes such as:
-
Missing crucial patient or prescription details.
-
Omitting the prescriber's signature.
-
Failing to provide clinical rationale where needed.
To avoid these pitfalls, it is advisable to review and validate all information carefully before submission. Double-checking entries can help ensure the form is processed without delays.
Security and Compliance for the Pharmacy Prior Authorization Request Form
The protection of sensitive information in the Pharmacy Prior Authorization Request Form is paramount. Compliance with standards such as HIPAA and GDPR ensures that patient data remains secure throughout the process.
pdfFiller employs extensive security measures, including 256-bit encryption, to safeguard the integrity of sensitive documents during handling and storage. These protocols help maintain confidentiality and trust in using digital forms.
What Happens After You Submit the Pharmacy Prior Authorization Request Form?
Once the Pharmacy Prior Authorization Request Form has been submitted, it undergoes processing within the designated timeframe. Applicants will typically receive updates regarding the status of their submission, which helps them stay informed.
Tracking submission status is essential for timely follow-up on any inquiries or additional information requests from the authority reviewing the form. This proactive approach can help address issues swiftly.
Streamline Your Pharmacy Prior Authorization Process with pdfFiller
Leveraging pdfFiller’s capabilities can significantly simplify the Pharmacy Prior Authorization Request Form process. Users benefit from an intuitive interface designed for ease of use, supported by robust security features and responsive customer support.
Utilizing pdfFiller can facilitate quicker form completion and submission, ultimately improving the efficiency of the prior authorization process for healthcare providers and their patients.
How to fill out the Cigna Uniform Pharmacy Prior Authorization Request
-
1.Access pdfFiller and search for the Pharmacy Prior Authorization Request Form using the search bar.
-
2.Select the form to open it in the editor. Familiarize yourself with the fillable fields available within pdfFiller's interface.
-
3.Gather necessary information including patient details, prescriber information, medication name, dosage, and clinical rationale for the prescription.
-
4.Begin filling out the form, starting with the patient’s full name, address, and date of birth in the designated fields.
-
5.Continue by entering the prescriber’s information including their name, contact details, and any necessary identification numbers.
-
6.Fill in the drug information, including medication name, dosage, and frequency, along with any clinical criteria needed for approval.
-
7.Review all entered information carefully, ensuring accuracy in all fields to prevent any issues during submission.
-
8.Use the pdfFiller toolbar to save your progress regularly and utilize the preview function to see a final version of the completed form.
-
9.Once satisfied with the filled form, either download it as a PDF for printing or submit it directly via email or fax as instructed on the form.

Who is eligible to use the Pharmacy Prior Authorization Request Form?
The form is intended for healthcare providers, specifically prescribers who require prior authorization for prescription medications on behalf of their patients.
What supporting documents should accompany the form?
Typically, supporting documents include medical records, treatment history, and any clinical criteria that justify the need for prior authorization, although specific requirements may vary by insurer.
How do I submit the form once completed?
After filling out the form, you can submit it through pdfFiller directly via email, or print and fax it to the designated contact number provided on the form.
Are there deadlines for submitting this form?
Deadlines vary depending on the insurance provider, so it's best to check their specific requirements to avoid any delays in medication approval.
What are common mistakes to avoid when filling out this form?
Be careful to enter accurate patient and prescriber information, double-check the medication details, and ensure required fields are filled to prevent processing delays.
How long does it take to process a prior authorization request?
Processing times can vary but usually take several days. Contact the specific insurance provider for estimated turnaround times.
Do I need to notarize the Pharmacy Prior Authorization Request Form?
No, notarization is not required for this form; however, it must be signed by the prescriber to be valid.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.