
Get the free Medicare Medical Savings Account (MSA) Plans
Show details
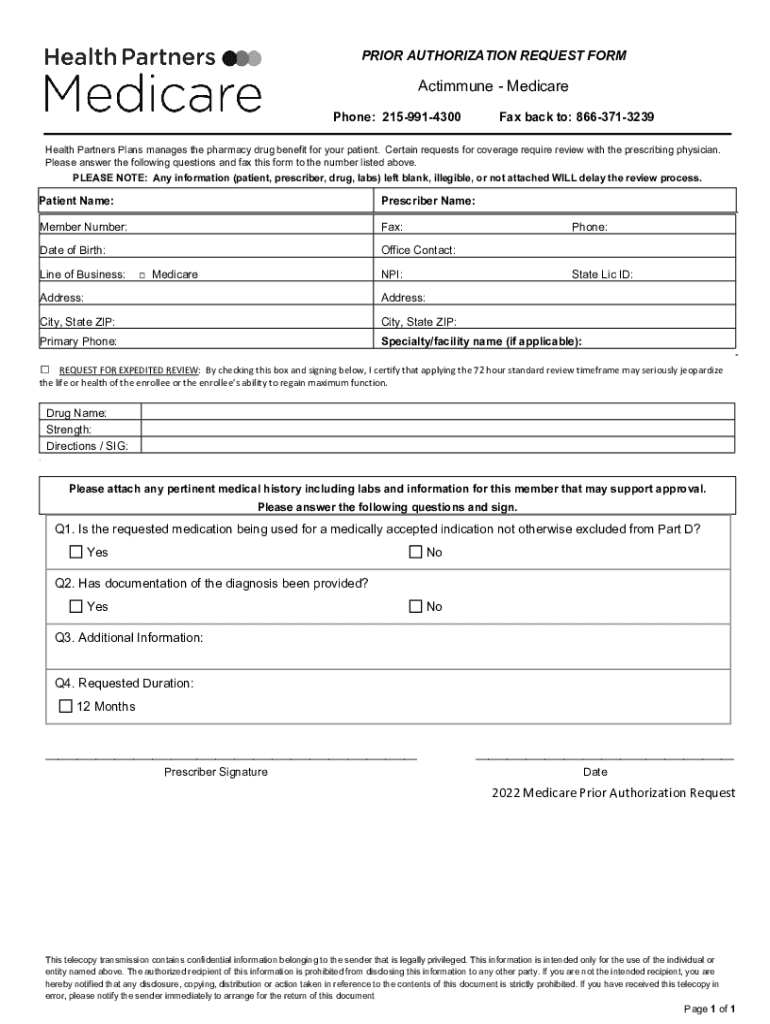
PRIOR AUTHORIZATION REQUEST FORMActimmune Medicare Phone: 2159914300Fax back to: 8663713239Health Partners Plans manages the pharmacy drug benefit for your patient. Certain requests for coverage require
We are not affiliated with any brand or entity on this form
Get, Create, Make and Sign medicare medical savings account
Edit your medicare medical savings account form online
Type text, complete fillable fields, insert images, highlight or blackout data for discretion, add comments, and more.
Add your legally-binding signature
Draw or type your signature, upload a signature image, or capture it with your digital camera.

Share your form instantly
Email, fax, or share your medicare medical savings account form via URL. You can also download, print, or export forms to your preferred cloud storage service.
Editing medicare medical savings account online
To use the professional PDF editor, follow these steps below:
1
Set up an account. If you are a new user, click Start Free Trial and establish a profile.
2
Upload a document. Select Add New on your Dashboard and transfer a file into the system in one of the following ways: by uploading it from your device or importing from the cloud, web, or internal mail. Then, click Start editing.
3
Edit medicare medical savings account. Replace text, adding objects, rearranging pages, and more. Then select the Documents tab to combine, divide, lock or unlock the file.
4
Get your file. Select your file from the documents list and pick your export method. You may save it as a PDF, email it, or upload it to the cloud.
It's easier to work with documents with pdfFiller than you can have ever thought. You may try it out for yourself by signing up for an account.
Uncompromising security for your PDF editing and eSignature needs
Your private information is safe with pdfFiller. We employ end-to-end encryption, secure cloud storage, and advanced access control to protect your documents and maintain regulatory compliance.
How to fill out medicare medical savings account
How to fill out medicare medical savings account
01
Determine if you are eligible for a Medicare Medical Savings Account (MSA)
02
Enroll in a high-deductible Medicare Advantage Plan that offers a Medical Savings Account
03
Make sure you have both Medicare Part A and Part B
04
Contribute to your MSA account with tax-free funds that can be used for medical expenses
05
Keep track of your MSA account balance and expenses to ensure proper usage
Who needs medicare medical savings account?
01
Individuals who have a high-deductible Medicare Advantage Plan and are looking for a way to save for medical expenses
02
People who want to take advantage of tax-free funds for healthcare costs
Fill
form
: Try Risk Free






For pdfFiller’s FAQs
Below is a list of the most common customer questions. If you can’t find an answer to your question, please don’t hesitate to reach out to us.
How can I send medicare medical savings account to be eSigned by others?
medicare medical savings account is ready when you're ready to send it out. With pdfFiller, you can send it out securely and get signatures in just a few clicks. PDFs can be sent to you by email, text message, fax, USPS mail, or notarized on your account. You can do this right from your account. Become a member right now and try it out for yourself!
How do I fill out the medicare medical savings account form on my smartphone?
You can quickly make and fill out legal forms with the help of the pdfFiller app on your phone. Complete and sign medicare medical savings account and other documents on your mobile device using the application. If you want to learn more about how the PDF editor works, go to pdfFiller.com.
Can I edit medicare medical savings account on an iOS device?
Create, modify, and share medicare medical savings account using the pdfFiller iOS app. Easy to install from the Apple Store. You may sign up for a free trial and then purchase a membership.
What is medicare medical savings account?
A Medicare Medical Savings Account (MSA) is a type of Medicare plan that combines a high-deductible health insurance plan with a medical savings account. Beneficiaries can use the money in the account to pay for qualified medical expenses.
Who is required to file medicare medical savings account?
Individuals who have a Medicare Medical Savings Account must file Form 8853 to report contributions and distributions related to their MSA.
How to fill out medicare medical savings account?
To fill out the Medicare Medical Savings Account, use Form 8853, provide information about contributions and distributions, and report any gains or losses on the account to the IRS.
What is the purpose of medicare medical savings account?
The purpose of a Medicare Medical Savings Account is to provide a tax-advantaged way for Medicare beneficiaries to save for and manage their medical expenses.
What information must be reported on medicare medical savings account?
The information that must be reported includes the total contributions made to the MSA, the distributions taken from the MSA, and any contributions made by the employer.
Fill out your medicare medical savings account online with pdfFiller!
pdfFiller is an end-to-end solution for managing, creating, and editing documents and forms in the cloud. Save time and hassle by preparing your tax forms online.

Medicare Medical Savings Account is not the form you're looking for?Search for another form here.
Relevant keywords
Related Forms
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.





















