Last updated on Sep 10, 2015

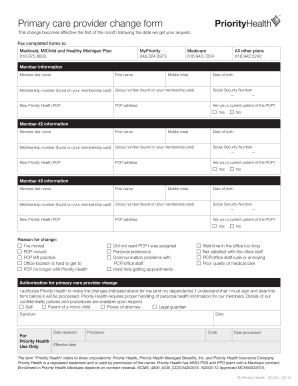
Get the free Priority Health Medicare Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Medicare Prior Authorization
The Priority Health Medicare Prior Authorization Form is a medical document used by healthcare providers to request prior authorization for the prescription drug Nexavar under Medicare.
pdfFiller scores top ratings on review platforms




Who needs Medicare Prior Authorization?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Medicare Prior Authorization
What is the Priority Health Medicare Prior Authorization Form?
The Priority Health Medicare Prior Authorization Form is a critical document utilized for obtaining prior authorization for the prescription drug Nexavar (sorafenib) under Medicare Part B or Part D. This form facilitates the request process by providing necessary details required from both the member and the provider. It captures essential information, such as patient identification and the medically accepted indication for the medication. Understanding its role is vital for healthcare providers and patients alike to ensure correct submissions.
Purpose and Benefits of the Priority Health Medicare Prior Authorization Form
The main purpose of the Priority Health Medicare Prior Authorization Form is to expedite the approval process for necessary medications. By using this specialized form, healthcare providers can ensure compliance with Medicare guidelines, which is crucial for securing coverage. Another significant advantage is the potential cost savings for patients, as proper authorization can lead to guaranteed coverage for prescribed treatments.
Key Features of the Priority Health Medicare Prior Authorization Form
This form includes several essential features designed to assist users. The fillable format allows for efficient data entry, requiring key fields such as:
-
Patient information including last name and date of birth.
-
Provider details for authorization validation.
-
Check boxes for indicating specific conditions.
Furthermore, clear instructions are provided to ensure that all submissions are legible and complete, enhancing the chances of successful approval.
Who Needs to Use the Priority Health Medicare Prior Authorization Form?
The Priority Health Medicare Prior Authorization Form is primarily utilized by healthcare providers seeking authorization on behalf of their patients. Any healthcare professional who prescribes medication that requires prior authorization should be familiar with this form. Specific scenarios that necessitate its use may include prescriptions for high-cost medications or those not routinely covered under Medicare.
When and How to Submit the Priority Health Medicare Prior Authorization Form
Submitting the Priority Health Medicare Prior Authorization Form should be done timely, particularly when a patient requires medication urgently. Here’s a step-by-step guide on how to fill out the form and submit it:
-
Access the form online using the pdfFiller platform.
-
Enter the required patient and provider information accurately.
-
Ensure all fields are complete and legible.
-
Submit the completed form via fax to Priority Health.
Be mindful of any deadlines associated with the medication needs and check for potential submission fees.
Common Errors and Validation Checklist for the Priority Health Medicare Prior Authorization Form
To ensure a successful submission of the form, users should be aware of common mistakes that could delay processing. Common errors include:
-
Missing patient or provider signatures.
-
Incomplete or illegible fields.
A validation checklist prior to submission can help confirm all necessary information is correctly filled out. It’s essential to review the form thoroughly to avoid setbacks.
Security and Compliance When Using the Priority Health Medicare Prior Authorization Form
Security in handling the Priority Health Medicare Prior Authorization Form is paramount. The use of pdfFiller ensures compliance with regulations such as HIPAA and GDPR through robust security features, including 256-bit encryption. Healthcare providers must also prioritize patient privacy by safeguarding all submitted information throughout the request process.
How pdfFiller Can Simplify Your Experience with the Priority Health Medicare Prior Authorization Form
pdfFiller offers several tools that can enhance the user experience when completing the Priority Health Medicare Prior Authorization Form. With its cloud-based platform, users can edit and fill out forms easily, ensuring both accuracy and efficiency in form completion. The capability to access documents on-the-go allows for timely updates, thereby streamlining the authorization process.
What Happens After Submission of the Priority Health Medicare Prior Authorization Form?
After submitting the Priority Health Medicare Prior Authorization Form, users should be prepared for the follow-up process. Typical timelines for approval can vary, and it is crucial to track the submission status. In case additional information is requested or if there is a rejection, understanding the necessary next steps can greatly assist in resolving any issues.
Engage with pdfFiller to Successfully Complete Your Priority Health Medicare Prior Authorization Form
Using pdfFiller ultimately simplifies the journey of completing the Priority Health Medicare Prior Authorization Form. The platform’s user-friendly features ensure an efficient and secure experience. Users are encouraged to take advantage of pdfFiller’s tools by starting their free trial or logging in today to manage their healthcare documents with confidence.
How to fill out the Medicare Prior Authorization
-
1.Access the Priority Health Medicare Prior Authorization Form on pdfFiller by searching its name in the platform's search bar or by using the provided link.
-
2.Once opened, familiarize yourself with the fields, which include patient information, prescribing provider details, and drug specifics.
-
3.Begin by filling out the patient's last name, first name, ID number, and date of birth in the relevant fields to ensure clear identification.
-
4.Next, enter your information as the requesting provider, including your name and signature, ensuring you provide a legible entry.
-
5.Gather necessary medical documentation, including the medically accepted indication for Nexavar, to support the request.
-
6.Ensure all sections of the form are filled completely and legibly, as incomplete forms may delay the review process.
-
7.Once all fields are completed, review the information for accuracy, focusing on spelling and completeness to avoid common errors.
-
8.Use pdfFiller's options to save your progress or make any necessary edits before finalizing the document.
-
9.Finally, submit the completed form by faxing it to Priority Health, using the fax number provided in the instructions available within the form.

What are the eligibility requirements for using this form?
To use the Priority Health Medicare Prior Authorization Form, the patient must have Medicare coverage and be prescribed Nexavar by a qualified healthcare provider. Ensure the medication request aligns with Medicare's guidelines.
What is the submission procedure for this form?
Complete the form in its entirety and ensure it is signed by the requesting provider. The final step is to fax the completed form to Priority Health for review to ensure it is processed correctly.
What supporting documents are required with this form?
You may need to attach medical records or documentation that verifies the medical necessity for prescribing Nexavar. Ensure all supporting documents are organized and legible for quicker processing.
What common mistakes should be avoided when filling this form?
Avoid submitting with incomplete fields, illegible handwriting, or missing signatures. Double-check that all required personal and medical information is filled accurately.
How long does it take to process a prior authorization request?
Processing times can vary but usually take a few days to a week. Ensure all necessary information is submitted to avoid delays in receiving approval.
Are there any fees associated with submitting this form?
Typically, there are no fees directly associated with submitting the Priority Health Medicare Prior Authorization Form. However, check with your healthcare provider or insurance representative for any potential costs.
Can this form be completed electronically?
Yes, the Priority Health Medicare Prior Authorization Form can be completed electronically using pdfFiller. This allows for easy filling, editing, and submission directly through the platform.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.