Last updated on Sep 10, 2015

Get the free Priority Health Medicare Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Medicare Prior Authorization
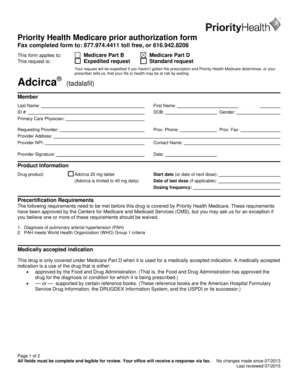
The Priority Health Medicare Prior Authorization Form is a healthcare document used by requesting providers to seek prior authorization for the drug Beleodaq under Medicare Part B and Part D.
pdfFiller scores top ratings on review platforms




Who needs Medicare Prior Authorization?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Medicare Prior Authorization
What is the Priority Health Medicare Prior Authorization Form?
The Priority Health Medicare Prior Authorization Form is a crucial document used in the healthcare process to request prior authorization for specific medications. This form is essential for obtaining drug approvals under Medicare, ensuring that necessary treatments are accessible to patients. By facilitating the authorization process, healthcare providers can better manage patient care while adhering to Medicare regulations.
This form holds significant importance as it directly impacts a patient's ability to receive prescribed medications, making it a vital component in the healthcare workflow.
Purpose and Benefits of the Priority Health Medicare Prior Authorization Form
The purpose of the Priority Health Medicare Prior Authorization Form is to streamline the process of obtaining necessary medications, particularly under Medicare Part B and Part D. Effective prior authorization ensures that patients receive the appropriate medications while adhering to Medicare coverage guidelines.
-
Ensures coverage for critical medications.
-
Prevents claim denials by meeting Medicare's criteria.
-
Facilitates communication between providers and insurers.
Essential Information Required on the Priority Health Medicare Prior Authorization Form
Filling out the Priority Health Medicare Prior Authorization Form requires specific information to ensure accuracy and compliance. Key details include:
-
Patient details such as name, ID number, and date of birth.
-
Drug product information including dosage and frequency.
-
Requesting provider details, including contact information and NPI.
Fields like "Requesting Provider" and "Drug Product" are crucial for correctly processing the authorization request.
How to Fill Out the Priority Health Medicare Prior Authorization Form Online
To complete the Priority Health Medicare Prior Authorization Form electronically, follow these steps:
-
Access the form via the designated online platform.
-
Input patient and provider information accurately.
-
Fill in the drug product details, including dosing information.
-
Review all sections for completeness and accuracy.
-
Submit the form electronically according to the instructions provided.
Ensure you double-check each field to avoid common errors during submission.
Common Errors to Avoid When Submitting the Priority Health Medicare Prior Authorization Form
When submitting the Priority Health Medicare Prior Authorization Form, certain mistakes can lead to delays or rejections:
-
Incomplete patient or provider information.
-
Incorrect drug product details or dosing frequency.
-
Failure to sign or date the form where required.
To mitigate these issues, always review the form thoroughly before submission and follow any specific guidelines provided by Priority Health.
Submission Methods for the Priority Health Medicare Prior Authorization Form
Submitting the Priority Health Medicare Prior Authorization Form can be accomplished through various methods. Generally, the completed form is submitted via fax:
-
Ensure the submission is sent to the correct fax number.
-
Consider keeping a copy of the fax confirmation for your records.
Adhere to any additional submission guidelines to ensure your request is reviewed promptly.
What Happens After You Submit the Priority Health Medicare Prior Authorization Form?
After submitting the Priority Health Medicare Prior Authorization Form, the review process begins. Typically, the timeframe for reviewing the request can vary:
-
Expect communication regarding the status of your submission.
-
Tracking the submission may be possible through your provider account.
Understanding this process helps in anticipating the next steps and potential outcomes.
Security and Compliance Considerations for the Priority Health Medicare Prior Authorization Form
When handling the Priority Health Medicare Prior Authorization Form, it is essential to understand security and compliance considerations. Secure document handling is paramount to protect sensitive patient information.
Compliance with standards such as HIPAA and GDPR ensures that data privacy is prioritized during submission and processing.
Utilizing pdfFiller to Complete the Priority Health Medicare Prior Authorization Form
pdfFiller offers valuable features for users looking to fill out the Priority Health Medicare Prior Authorization Form efficiently. Its capabilities include:
-
Editing text and images directly within the PDF.
-
Creating fillable forms to streamline the data entry process.
-
eSigning documents securely, ensuring compliance.
These features allow users to manage their forms effectively while ensuring security and ease of use.
Getting Started with the Priority Health Medicare Prior Authorization Form
To begin using the Priority Health Medicare Prior Authorization Form, take advantage of pdfFiller for a seamless experience. The platform provides an efficient way to complete healthcare forms, making the process straightforward and user-friendly.
With pdfFiller, you can navigate the complexities of healthcare documentation with confidence and security.
How to fill out the Medicare Prior Authorization
-
1.Access pdfFiller and search for the Priority Health Medicare Prior Authorization Form in the templates section.
-
2.Open the form by clicking on it to start editing within the pdfFiller interface.
-
3.Before starting, gather necessary information such as patient details, requesting provider information, and specific drug product information.
-
4.Begin filling out the form by entering the patient's last name, first name, ID number, and date of birth in the designated fields.
-
5.Continue by filling out additional details like gender, primary care physician, provider contact information, and provider NPI number.
-
6.Complete any required fields indicating the dose, dosing frequency, patient’s body surface area, CPT codes, and checkmarking any 'Yes' or 'No' options if applicable.
-
7.Once all fields are filled out, review the input information for accuracy and completeness to avoid common mistakes.
-
8.Finalize the form by saving your progress on pdfFiller, ensuring you retain a copy for your records.
-
9.Download the completed form or submit it directly through pdfFiller by following the on-screen prompts, including faxing if required.

Who is eligible to use the Priority Health Medicare Prior Authorization Form?
The Priority Health Medicare Prior Authorization Form is primarily for healthcare providers seeking approval for Medicare drugs on behalf of their patients. Patients enrolled in Medicare can also provide their provider with required details to facilitate the process.
What documents do I need to submit with this form?
Typically, you may need to submit supporting documents such as the patient's Medicare details, prior medical records, and information about the drug requesting approval. Check with Priority Health for specific requirements.
How do I submit the completed form?
You can submit the completed Priority Health Medicare Prior Authorization Form by faxing it to Priority Health. Ensure all required fields are accurately filled out to avoid delays in processing.
What common mistakes should I avoid when filling out this form?
Common mistakes include leaving fields blank, entering incorrect patient or provider information, and not checking the necessary boxes for 'Yes' or 'No' responses. Double-check your entries before submission.
Is there a processing time for the submission of this form?
Processing times can vary, but generally, expect to receive a response within a few business days after submitting your authorization request. Check Priority Health guidelines for detailed timelines.
Are there any fees associated with this authorization process?
As of my last update, there are typically no fees for processing the Medicare prior authorization request itself. However, patients should verify if any associated costs exist with the medication or services required.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.