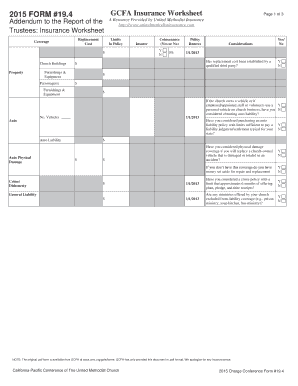
Last updated on Sep 10, 2015

Get the free Priority Health Medicare Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Medicare Prior Authorization
The Priority Health Medicare Prior Authorization Form is a medical consent document used by healthcare providers to request prior authorization for the drug Xtandi under Medicare.
pdfFiller scores top ratings on review platforms




Who needs Medicare Prior Authorization?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Medicare Prior Authorization
What is the Priority Health Medicare Prior Authorization Form?
The Priority Health Medicare Prior Authorization Form is essential for healthcare providers seeking prior authorization for medications, particularly the drug Xtandi (enzalutamide) under Medicare. This form plays a critical role in managing treatment approvals, ensuring that patients receive necessary medications without unnecessary delays.
The form, which was last reviewed in July 2015, holds significant implications for the authorization process, particularly regarding the information required for approval and the potential impact on patient care.
Purpose and Benefits of the Priority Health Medicare Prior Authorization Form
Obtaining prior authorization for certain medications, such as Xtandi, is vital for compliance with Medicare requirements. The form facilitates a smoother process for both healthcare providers and patients, ultimately enhancing the efficiency of medication management.
Properly completing this form can help prevent treatment delays, ensuring that patients start their necessary therapies in a timely manner, thus improving health outcomes.
Key Features of the Priority Health Medicare Prior Authorization Form
This form includes several fillable fields that collect critical patient and treatment information, including:
-
Patient details such as name, date of birth, and ID number
-
Medication specifics including drug product, dosing frequency, and start dates
-
Clinical information like ECOG status and PSA levels
-
Provider information, including signature and contact details
Each section is designed to ensure that healthcare providers submit comprehensive and accurate information required for the authorization process.
Who Needs the Priority Health Medicare Prior Authorization Form?
Healthcare providers are the primary users of this form as they submit requests for prior authorization. Patients who require Xtandi also must have this form completed to navigate the Medicare process effectively.
In addition, other stakeholders involved in Medicare may need to reference this form to understand the requirements attached to prior authorization requests.
How to Fill Out the Priority Health Medicare Prior Authorization Form Online (Step-by-Step)
To complete the Priority Health Medicare Prior Authorization Form online, follow these steps:
-
Gather all necessary patient information beforehand, including personal and clinical details.
-
Fill in the patient and provider sections accurately, ensuring all required fields are completed.
-
Double-check the clinical information, particularly ECOG status and PSA levels for accuracy.
-
Submit the form electronically through the prescribed submission channel.
Be aware of common mistakes, such as missing signatures or incomplete sections, which can lead to delays in processing.
Submission Methods and Delivery: Where to Submit the Priority Health Medicare Prior Authorization Form
Once completed, the Priority Health Medicare Prior Authorization Form can be submitted via various methods, including:
-
Faxing to the designated Medicare office
-
Online uploading through the appropriate portal
It is important to note any potential submission fees and the expected processing times. Late or incorrect submissions can result in denied requests, complicating patient care.
Common Errors and How to Avoid Them
Common pitfalls when filling out the Priority Health Medicare Prior Authorization Form include:
-
Leaving sections incomplete or unclear, particularly clinical details.
-
Failing to include the provider's signature, which is required for processing.
To mitigate these issues, double-check your entries for accuracy and completeness before submitting, and securely document any submission confirmations.
Security and Compliance for the Priority Health Medicare Prior Authorization Form
When handling sensitive patient information, security and compliance are paramount. pdfFiller employs robust measures, including 256-bit encryption and HIPAA compliance, to ensure document security throughout the submission process.
Maintaining patient confidentiality is crucial, and users must adhere to these data protection measures to safeguard sensitive information.
Sample or Example of a Completed Priority Health Medicare Prior Authorization Form
To assist users in understanding how to complete the form correctly, a visual representation of a filled-out Priority Health Medicare Prior Authorization Form is available. This example includes annotations that explain each section of the form clearly.
Users can also find download or print options through pdfFiller to access this resource conveniently.
Why Choose pdfFiller for Your Medicare Prior Authorization Needs?
pdfFiller offers a user-friendly platform that simplifies the process of completing and managing the Priority Health Medicare Prior Authorization Form. Key benefits include:
-
Editable form capabilities that allow users to tailor documents easily
-
eSigning features that streamline approvals and sign-offs
-
Positive feedback from healthcare providers who have improved their efficiency with pdfFiller
Choosing pdfFiller means leveraging a powerful tool designed for managing essential healthcare documentation efficiently and securely.
How to fill out the Medicare Prior Authorization
-
1.Access the Priority Health Medicare Prior Authorization Form on pdfFiller by searching its name or selecting it from your documents list.
-
2.Open the document in the pdfFiller interface to view all fillable fields.
-
3.Before starting, gather essential patient information: diagnosis, ECOG status, PSA levels, serum testosterone levels, and provider details.
-
4.Click on each field to begin filling in necessary information: 'Last Name', 'First Name', 'ID #', and so on.
-
5.Ensure to accurately complete sections requiring justification for the prior authorization, including specific patient conditions and treatment justifications.
-
6.Use pdfFiller's tools to check for errors or incomplete fields once all information is entered.
-
7.Review the completed form thoroughly to ensure all provided details are correct and complete.
-
8.Finalize your document by saving it as a PDF or directly downloading it in your preferred format.
-
9.If required, submit the completed form to the appropriate insurance provider or regulatory body as instructed.

What are the eligibility requirements for submitting the Prior Authorization Form?
Eligibility typically requires that the patient is enrolled in Medicare and that the Xtandi prescription is medically necessary per Medicare guidelines.
Are there deadlines for submitting the Prior Authorization Form?
Yes, it is advised to submit the Prior Authorization Form as soon as the prescription is written to avoid delays in medication access for the patient.
How do I submit the Form after completing it?
The completed form can be submitted electronically via fax or mail, depending on the instructions provided by the insurance company.
What supporting documents are needed with this Prior Authorization Form?
Typically required documents include the patient's medical records, a letter of medical necessity, and any relevant lab results to support the prior authorization request.
What common mistakes should I avoid when filling out the form?
Ensure that all fields are accurately filled out, particularly patient identifiers and medical details; missing or incorrect information can delay processing.
How long does it take to process the Prior Authorization Form?
Processing times can vary, but most insurance providers aim to respond within 5-14 business days after receipt of the completed form.
What should I do if my initial request is denied?
If denied, review the denial reasons provided, gather additional documentation if needed, and consider filing an appeal to support the prior authorization.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.