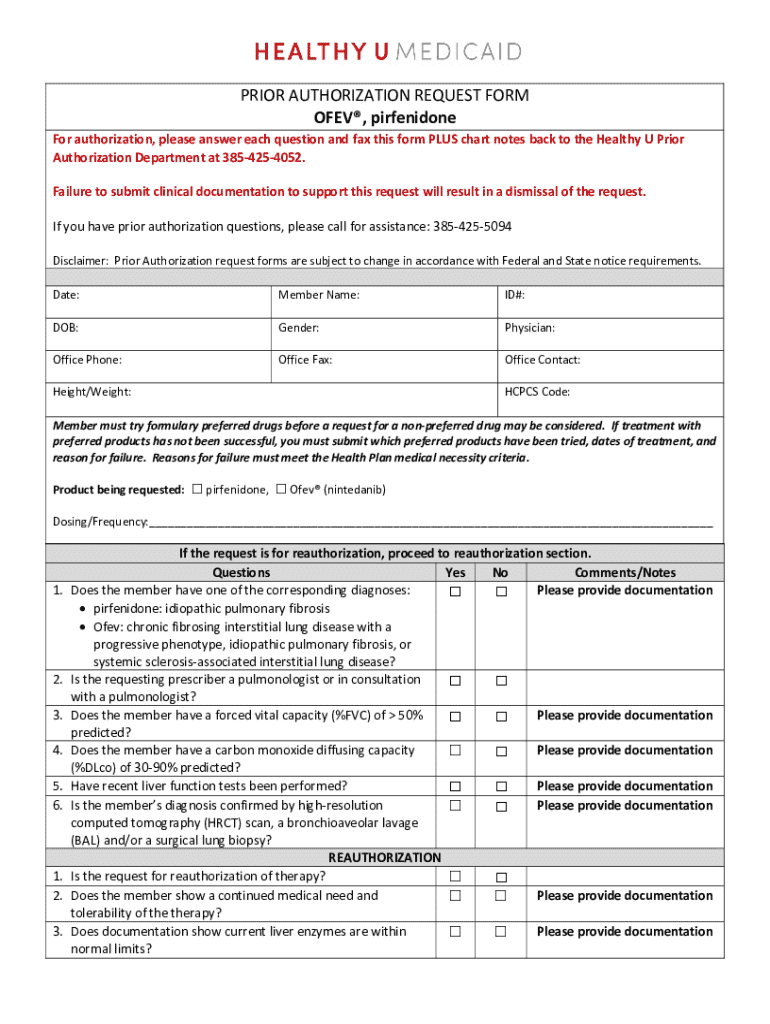

Get the free PRIOR AUTHORIZATION REQUEST FORM ACNE ...
Get, Create, Make and Sign prior authorization request form

Editing prior authorization request form online
Uncompromising security for your PDF editing and eSignature needs
How to fill out prior authorization request form
How to fill out prior authorization request form
Who needs prior authorization request form?
A Comprehensive Guide to Prior Authorization Request Forms
Understanding prior authorization
Prior authorization is a critical process in the healthcare system that requires healthcare providers to obtain approval from an insurance company before a patient can receive specific medications or procedures. This process ensures that the treatments prescribed are medically necessary and align with the patient's coverage plans.
The primary purpose of prior authorization is to manage healthcare costs, prevent misuse of resources, and promote appropriate care. Often, high-cost medications or procedures necessitate this approval to avoid unnecessary financial burdens on patients and insurance providers alike.
Importance of prior authorization request forms
A prior authorization request form is an essential tool used by healthcare providers to initiate the authorization process. This standardized document collects necessary information about the patient’s condition and the requested treatment, ensuring a clear and efficient communication pathway between the provider and the insurance company.
Utilizing a prior authorization request form offers several benefits: it streamlines the communication process, reduces the likelihood of missing information that could delay approval, and enhances the chances of obtaining timely authorization for necessary treatments.
Key components of the prior authorization request form
Understanding the components of a prior authorization request form is critical to its successful completion. Each section has its purpose and must be filled out carefully to ensure accuracy.
Steps to complete the prior authorization request form
Completing a prior authorization request form involves several steps to ensure a smooth process. Failing to follow these steps may result in delays or denials, making meticulous attention to detail crucial.
Common challenges with prior authorization requests
While essential, the prior authorization process is fraught with challenges that can complicate patient care. Providers often encounter various issues that can lead to frustration.
Interactive tools for managing prior authorization requests
Utilizing modern tools like pdfFiller can significantly simplify managing prior authorization request forms. This platform not only allows users to create and edit necessary documentation but also enhances collaboration among healthcare teams.
FAQs about prior authorization requests
An informed approach to handling prior authorization requests can ease the process for both providers and patients. Here are some frequently asked questions that can guide users.
Case studies and success stories
Real-life examples of successful prior authorization requests can serve as powerful motivators for best practices. Understanding what worked in these scenarios can guide others toward similar success.
Additionally, examining denial cases can shed light on common pitfalls. Identifying these issues allows providers to take proactive measures to avoid them in future requests.
Keeping your prior authorization request form up-to-date
Staying current with your prior authorization request form is essential. Regular updates ensure that both patient data and treatment information are accurate, which is crucial for gaining speedy approvals.
Conclusion: navigating prior authorization with ease
Navigating the world of prior authorization can seem daunting, but with the right tools and mindset, it can be managed effectively. Platforms like pdfFiller simplify this process, assisting users in creating, editing, collaborating, and managing all necessary documentation seamlessly.
By leveraging digital solutions, healthcare professionals can improve their document management workflows, lessen the burden of administrative tasks, and ultimately focus more on patient care.






For pdfFiller’s FAQs
Below is a list of the most common customer questions. If you can’t find an answer to your question, please don’t hesitate to reach out to us.
How can I send prior authorization request form for eSignature?
Where do I find prior authorization request form?
How do I make edits in prior authorization request form without leaving Chrome?
What is prior authorization request form?
Who is required to file prior authorization request form?
How to fill out prior authorization request form?
What is the purpose of prior authorization request form?
What information must be reported on prior authorization request form?
pdfFiller is an end-to-end solution for managing, creating, and editing documents and forms in the cloud. Save time and hassle by preparing your tax forms online.















