Last updated on Oct 22, 2015

Get the free Pharmacy Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prior Authorization Form
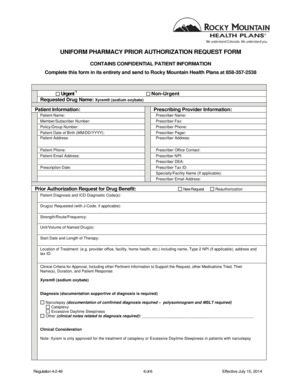
The Pharmacy Prior Authorization Request Form is a medical document used by healthcare providers to request prior authorization for the drug Kyprolis® for patients with relapsed multiple myeloma.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Form
What is the Pharmacy Prior Authorization Request Form?
The Pharmacy Prior Authorization Request Form is a crucial document for securing authorization for Kyprolis® (carfilzomib), specifically tailored for patients undergoing treatment for relapsed multiple myeloma. This form is vital as it ensures the necessary approvals from insurance providers, enabling healthcare providers to access treatment options in a timely manner. Understanding the role of Kyprolis® in managing multiple myeloma is essential, as it addresses the complexities involved in treating this condition. Furthermore, this form is closely associated with Rocky Mountain Health Plans, which facilitates patient access to necessary therapies.
Purpose and Benefits of the Pharmacy Prior Authorization Request Form
Utilizing the Pharmacy Prior Authorization Request Form streamlines the authorization process, ultimately leading to quicker treatment for patients. This form plays a pivotal role in ensuring compliance with the medical insurance requirements essential for administering Kyprolis®. Additionally, it fosters effective communication between prescribers and insurance companies, making it easier to navigate the healthcare landscape.
Who Needs the Pharmacy Prior Authorization Request Form?
The Pharmacy Prior Authorization Request Form is predominantly used by prescribers responsible for filling out this documentation. A prescriber, typically a licensed medical professional, must complete and sign the form to initiate the authorization process. Patients eligible for Kyprolis® must meet specific conditions that warrant the necessity of this form, emphasizing the critical role of the prescriber in ensuring accurate and timely submissions.
When to Submit the Pharmacy Prior Authorization Request Form
Timely submission of the Pharmacy Prior Authorization Request Form is essential to prevent treatment delays. There are specific criteria to determine when to file the request, often aligned with treatment schedules for multiple myeloma therapies. Failing to submit the form on time can lead to significant consequences, including interruptions in patient care, underscoring the importance of adhering to submission deadlines outlined in treatment protocols.
How to Fill Out the Pharmacy Prior Authorization Request Form Online
Completing the Pharmacy Prior Authorization Request Form online requires attention to detail in several key areas:
-
Patient details, including demographics and medical history.
-
Prescriber information, ensuring accuracy in contact details.
-
Clinical criteria that justify the authorization request.
Field-by-field guidance is essential in this process to avoid errors and enhance compliance. Additional tips include careful review of common sections and checkboxes to ensure the form's completeness and accuracy before submission.
Common Errors and How to Avoid Them
Users often encounter frequent mistakes that can lead to rejection or delays in processing the Pharmacy Prior Authorization Request Form. Common pitfalls include:
-
Incomplete patient or prescriber information.
-
Missing clinical justification details.
To mitigate these issues, best practices suggest reviewing the completed form thoroughly and ensuring the prescriber’s signature is present, confirming the document's validity.
How to Sign and Submit the Pharmacy Prior Authorization Request Form
Signing and submitting the Pharmacy Prior Authorization Request Form involves understanding both digital and wet signature requirements. Various efficient submission methods are available, including:
-
Online submission through the appropriate platform.
-
Faxing the completed form directly to Rocky Mountain Health Plans.
-
Mailing a physical copy if needed.
Choosing the optimal delivery method ensures that the request reaches the insurance provider without unnecessary delays.
Security and Compliance for the Pharmacy Prior Authorization Request Form
When handling sensitive patient information, security and compliance are paramount. The platform used for completing the Pharmacy Prior Authorization Request Form implements several robust security measures, including:
-
256-bit encryption for data protection.
-
Compliance with HIPAA and GDPR regulations.
Understanding these security protocols helps reassure users about the safety of their data during the form-filling and submission process.
Why Use pdfFiller for Your Pharmacy Prior Authorization Request Form Needs?
pdfFiller offers a reliable solution for handling the Pharmacy Prior Authorization Request Form effectively. Key features of pdfFiller include:
-
Cloud-based editing that allows users to work from any location.
-
User-friendly interface designed to simplify form completion.
Additionally, pdfFiller guarantees high standards of data privacy and security, making it a trustworthy option for healthcare professionals.
Get Started with Your Pharmacy Prior Authorization Request Form Today!
Utilizing the Pharmacy Prior Authorization Request Form is essential for facilitating treatment for multiple myeloma patients. pdfFiller aids in the processing of this vital document, streamlining the necessary procedures for prescribers and patients alike. Experience the benefits of easy document management and join the numerous users gaining value through pdfFiller’s intuitive platform.
How to fill out the Prior Authorization Form
-
1.To access the Pharmacy Prior Authorization Request Form on pdfFiller, open your browser and navigate to the pdfFiller website. Use the search bar to find the form by entering its name.
-
2.Once the form appears, click on it to open it in the interactive editor. You can zoom in or out for easier viewing as needed.
-
3.Before filling out the form, gather all relevant patient information such as diagnosis details, medication requests, and prescriber contact information.
-
4.Begin filling out the form by clicking on each blank field. Enter the required details including patient demographics, medical history, and any diagnosis codes related to the treatment.
-
5.Make sure to check the clinical criteria section and mark any applicable boxes to ensure all necessary information is included.
-
6.Once all the fields are completed, carefully review the entire form for accuracy. Ensure that all required signatures, particularly the prescriber’s signature, are present and clearly visible.
-
7.After reviewing, save your progress frequently to avoid losing any data. You can download the completed form in various formats, including PDF.
-
8.If ready to submit, follow the provided instructions for your specific insurance provider or print the form directly from pdfFiller for physical submission.

Who is eligible to use the Pharmacy Prior Authorization Request Form?
Any healthcare provider who prescribes Kyprolis® for patients with relapsed multiple myeloma is eligible to use this form. It is necessary to provide accurate patient information and prescriber details.
What information is needed to complete the form?
You will need detailed patient information, drug dosage requests, diagnosis codes, and clinical justifications. Ensure you have your signature and prescriber’s credentials ready.
How should the form be submitted?
Once completed, the form can be submitted directly to the patient's insurance provider, typically Rocky Mountain Health Plans. It is advisable to follow their specific submission guidelines.
Are there any deadlines for submitting the prior authorization request?
Deadlines may vary by insurance provider. It is crucial to check with the specific insurance company for their processing times and any timely submission requirements to avoid treatment delays.
Can this form be used for medications other than Kyprolis®?
No, this form is specifically designed for requesting prior authorization for Kyprolis® (carfilzomib) for patients with relapsed multiple myeloma. Other medications require their own specific forms.
What are common mistakes to avoid when filling out this form?
Common mistakes include incomplete patient information, missing prescriber signatures, and failing to double-check the accuracy of clinical criteria. Take your time to review all sections thoroughly.
How long does it take for the prior authorization to be processed?
Processing times can vary based on the insurance company. Typically, it can take several days to a few weeks, so early submission is advised to avoid delays in treatment.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.