Last updated on Mar 26, 2026

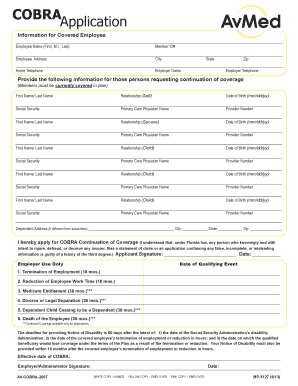
WageWorks COBRA Appeal Form free printable template
pdfFiller is not affiliated with any government organization
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is WageWorks COBRA Appeal Form
The COBRA Appeal Form is a health insurance document used by individuals to appeal the termination of their COBRA coverage.
pdfFiller scores top ratings on review platforms




Who needs WageWorks COBRA Appeal Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to WageWorks COBRA Appeal Form
What is the COBRA Appeal Form?
The COBRA Appeal Form is a crucial document for individuals seeking to contest the termination of their COBRA health coverage. This form acts as a safeguard for eligible participants, enabling them to maintain their healthcare benefits during challenging times. Participants play a key role in the appeal process by accurately completing the form and submitting it within the designated timeframe.
Purpose and Benefits of the COBRA Appeal Form
The form serves a significant purpose by helping individuals protect their health care coverage after a termination notice. It underscores the participant's right to appeal and potentially have their benefits reinstated. Utilization of the COBRA Appeal Form can lead to several advantages, including the reinstatement of previously lost health insurance coverage, thereby ensuring continued access to essential medical services.
Who Needs the COBRA Appeal Form?
The COBRA Appeal Form is intended for individuals who have experienced employment termination or a reduction in work hours that impacts their health insurance eligibility. Eligibility criteria typically include having been covered under a group health plan at the time of termination, as well as meeting the deadlines specified in the termination notice for the appeal. Recognizing these factors is important for participants looking to file an appeal.
How to Fill Out the COBRA Appeal Form Online
Completing the COBRA Appeal Form online involves several straightforward steps:
-
Access the form through a secure platform like pdfFiller.
-
Input personal information such as full name and address accurately.
-
Provide details regarding the termination, including dates and reasons.
-
Clearly state the reasons for your appeal in the designated section.
-
Review the completed form to ensure all fields are filled out correctly.
Required Documents and Supporting Materials
In addition to the COBRA Appeal Form, individuals are required to submit certain supporting documentation. This documentation may include:
-
The original termination notice received from the employer.
-
Copies of any relevant correspondence regarding the appeal.
-
Records of payments made for COBRA coverage, if applicable.
Gathering this documentation is essential as it significantly influences the outcome of the appeal by providing evidence to support the claim.
Submission Methods for the COBRA Appeal Form
Participants can submit the COBRA Appeal Form through various acceptable methods. Options include:
-
Online submission via a designated portal.
-
Mailing the completed form to the appropriate address as specified in your termination notice.
It is important to be aware of relevant deadlines; the appeal must generally be filed within 180 days of receiving the termination notice.
Common Errors and How to Avoid Them
Error-free completion of the COBRA Appeal Form is vital for a successful appeal. Common mistakes include:
-
Failing to sign the form where required.
-
Leaving out critical information or failing to provide sufficient details.
-
Missing the submission deadline.
To avoid these pitfalls, double-check each section of the form and follow the provided instructions carefully.
What Happens After Your COBRA Appeal Submission?
Once the COBRA Appeal Form is submitted, it undergoes a review process by an independent party. Participants can expect a decision typically within 30 days. Depending on the appeal's outcome, follow-up actions may include additional documentation requests or acknowledgment of the appeal's approval or denial.
Security and Privacy in Handling Your COBRA Appeal Form
Protecting personal health information is paramount when handling the COBRA Appeal Form. pdfFiller prioritizes security and complies with privacy regulations, ensuring that sensitive documents are safely processed. Utilizing their platform ensures that your personal data remains confidential and secure throughout the entire process.
Experience Hassle-Free Form Completion with pdfFiller
pdfFiller offers a user-friendly platform to fill out and submit the COBRA Appeal Form efficiently. With features like eSigning, form management, and enhanced document security, individuals can complete their appeals without unnecessary complications. Leverage pdfFiller's capabilities for a streamlined submission experience.
How to fill out the WageWorks COBRA Appeal Form
-
1.Access pdfFiller and log in to your account or create a new one if you don’t have one yet.
-
2.Use the search bar to find the 'COBRA Appeal Form' or browse through the Employment Forms category.
-
3.Once located, click on the form to open it in the editor where you will see fillable fields.
-
4.Gather all necessary personal information including your name, address, and details about the termination of your COBRA coverage before starting.
-
5.Navigate through the form fields and enter required information accurately, such as your personal details and reasons for the appeal.
-
6.Confirm all necessary financial details and any correspondence related to your coverage termination are filled in the relevant sections.
-
7.After filling in all fields, review the document carefully to ensure all information is correct and complete.
-
8.Utilize the review tool in pdfFiller to check for any missing fields or potential errors before finalizing.
-
9.Once satisfied, save your document and choose to download a copy for your records.
-
10.If you're ready to submit, follow the indicated process on pdfFiller to electronically submit your appeal, or download to mail it to the specified address.

Who is eligible to file the COBRA Appeal Form?
Individuals who have experienced a termination of their COBRA health insurance coverage are eligible to file this appeal. You must submit the form within 180 days of receiving a termination notice.
What is the deadline for submitting the COBRA Appeal Form?
The form must be submitted within 180 days following the receipt of the COBRA termination notice. Ensure you adhere to this timeline to have your appeal considered.
How do I submit the COBRA Appeal Form?
The COBRA Appeal Form can be submitted electronically through pdfFiller or printed and mailed directly to the appropriate address as outlined in the form instructions.
What supporting documents are required with the appeal?
You should include any relevant correspondence regarding the termination, proof of payments made towards your COBRA coverage, and any evidence supporting your argument for the appeal.
What are common mistakes to avoid when completing the form?
Ensure all fields are filled accurately and completely. Avoid missing any deadlines and double-check that all required supporting documents are included to avoid delays.
How long does it take to process the appeal?
Once submitted, the appeal is typically reviewed by an independent party, and you should receive a decision within 30 days. However, processing times may vary.
What should I do if my appeal is denied?
If your COBRA appeal is denied, you may request further explanation or consult legal advice for next steps. Ensure to keep copies of all communications.
Related Catalogs
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.